- Supply Chain
8 (mostly easy) ways to reduce your medical gas spend
As health systems continue to navigate tight margins and seek ways to transform variable expenses, there are some quick wins to be found. Step No. 1? Understand your product supply agreement.
- Clinical
- Supply Chain
Four ways to address ligature risks in patient rooms and beyond
Ligature risk mitigation requires collaboration among stakeholders and adherence to best practices, including comprehensive risk assessments, implementing design solutions, staff training, and ongoing monitoring and evaluation.
- Supply Chain
Tap into these four strategies to improve hospital water quality
To ensure patient safety, water quality is key. And there are four main strategies that can help achieve that goal: regular water quality testing, water treatment and technologies, equipment maintenance and calibration, and education and training.
- Supply Chain
One size does not fit all: The power of customer segmentation
In today’s highly competitive healthcare landscape, companies that embrace tailored segmentation approaches have witnessed significant gains in sales efficiency and profitability.
- Supply Chain
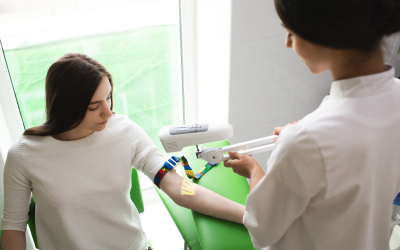
Vein Viewers Offer Benefits for Patients and Providers
The devices can reduce the discomfort and pain associated with multiple attempts at finding a vein and improve the accuracy and speed of vein location, reducing the need for repeat attempts or more invasive procedures.
- Clinical
- Operations & Quality
- Supply Chain
Improving the Provider Narrative: Vizient's Briefings Amplify the Voice of Hospitals on Capitol Hill
Learn about the three briefings that Vizient hosted in 2023 — attended by dozens of Congressional staff and Members of Congress — serving as a platform to remind policymakers of the critical impact of hospitals and health systems in their communities.
- Supply Chain
Three Areas Supply Chain Consultants Should Focus on to Help Hospitals Face Challenges
Cost management, technology adoption and inventory management solutions should be at the center of how supply chain consultants approach their work with hospitals, along with how those areas align with an organization’s specific needs and challenges.
- Supply Chain
Safety in Numbers: Strategies for PPE Inventory Management
How can health systems take a “Goldilocks” approach to PPE, ensuring they don’t have too much or too little – but rather, a “just right” amount that strikes a balance between financial and clinical requirements?
- Supply Chain
Enabling Successful Working Relationships Between Clinical Value Analysis and Purchasing Operations
The value of investing in relationships and combining strengths cannot be overstated when it comes to balance and collaboration in the healthcare supply chain, says Vizient’s Sam Weech.
- Supply Chain
Four Reasons Healthcare Organizations Should Implement Electric Vehicle Charging Infrastructure
As electric vehicle adoption continues to rise, hospitals can benefit from implementing EV charging infrastructure in many ways — financially, in their green initiatives, through data-driven insights, and in patient and employee satisfaction.
- Supply Chain
Creatively Reduce Costs in Healthcare Construction Projects
By leveraging performance improvement Group Purchasing Organizations (GPOs), healthcare organizations can optimize procurement and reduce project expenses in areas including materials, equipment and services.
- Supply Chain
Three Ways Sustainability Can Drive Immediate Cost Savings Across Health Systems
Strategies such as using clean, renewable energy, increasing reprocessing and recycling in the OR, and pursuing environmentally preferred purchasing can drive near-term savings across healthcare organizations, says Vizient’s Cristina Indiveri.
- Supply Chain
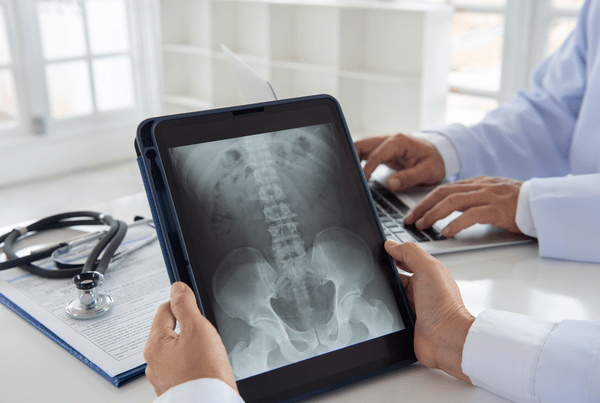
Are Radiology Detector Grids on the Brink of Obsolescence?
The healthcare community’s attention to radiation exposure has fueled the advent of newer technologies like digital detectors that offer the promise of reduced radiation exposure while maintaining diagnostic efficacy.
- Supply Chain
Balancing People, Technology for the Best Inventory Management Outcome
When we walk into a hospital, it's always interesting to see how inventory is managed in different departments.
- Supply Chain
- Data & Analytics
How Big Data Illuminates Social Drivers, Environmental Impacts and Patient Health
There is often a disconnect that exists between sustainability and health equity. Pinpointing the immense overlap between environmental impacts and social drivers of health is no easy feat, but data is key to helping providers see the bigger picture.
- Pharmacy
- Supply Chain
The Source of Truth: A Pharmacy Buyer’s Drug Shortage List
Drug shortages and their management have become a major focus of pharmacy staff within hospitals and health systems, which is why maintaining an institution-specific drug shortage list may be critical.
- Supply Chain
Shore Up Imaging Revenue During an Economic Downturn
Instead of reducing staffing levels if demand declines, forward-thinking health systems can maintain or increase volume through imaging associated with clinical research trials and firming up their referral base.
- Clinical
- Supply Chain
Ergonomics Should be of Paramount Importance to Gastroenterologists
While gastroenterologists are saving lives with vital endoscopy procedures, they need to be mindful of their own health and well-being, as poor body mechanics and improper ergonomics are negatively impacting their health, productivity and career longevity.
- Supply Chain
As Healthcare Continues to Evolve, Understanding the Cycle of Change is Crucial
The hospital supply chain and its leadership are in a state of volatile flux, meaning providers and their staff must adapt to meet new challenges and adjust to this new normal.
- Supply Chain
Take These Steps to Reduce Inventory Shrinkage in Your Hospital
From implementing strict inventory management procedures to establishing a culture of ownership, there are several quick-win approaches hospitals can take to ensure accurate inventory levels.
- Supply Chain
- Clinical
Safe Patient Handling Programs Reduce Risk, Increase Satisfaction
By reducing the risk of injury to healthcare workers, these programs can improve job satisfaction, decrease turnover and reduce healthcare costs associated with workers' compensation claims as well as improve patient outcomes.
- Data & Analytics
- Supply Chain
- Clinical
Using Contracting and Clinical Data Collaboratively to Gain Clinical and Executive Support
The key to effectively using supply spend, contract and clinical data is to correctly identify the need and expected result, as well as knowing the available data sources and tools to ensure the desired outcome can be achieved.
- Supply Chain
Your Technology Strategy is a C-suite Imperative
Health systems need a dual transformation — and the role of technology has never been more important in solving the problems of today and tomorrow.
- Supply Chain
Entering into a Medical IT Contract? Here are 7 Factors to Consider.
From looking at scope of work to dispute resolution clauses, there are several nuanced approaches hospitals can use to achieve success in contracting for information technology services and equipment.