By Cristina Indiveri, Vizient Associate Vice President, Core Tenet Programs
Heather Blonsky, Vizient Lead Data Scientist
It's a no-brainer that living next to a hazardous waste dump is harmful to human health. What's far more complex is understanding how poverty lands people in proximity to environmental hotspots — and how the absence of wealth, educational opportunities and access to care further exacerbate the risks that are already present.
Healthcare has long been accused of operating in silos and nowhere is that more apparent than in the disconnect that often exists between sustainability and health equity. Pinpointing the immense overlap between environmental impacts and social drivers of health is no easy feat, but it's a challenge that providers must nevertheless confront.
Data is the key to understanding the interconnectedness between the two — and ultimately driving positive action to improve human and environmental health.
How should I approach this crucial work?
One essential way to frame the importance of linking sustainability and health equity is through the lens of the CQO movement, which looks at the relationship between:
- Cost: The expenses associated with caring for individuals and communities.
- Quality: The care aimed at achieving the best possible health.
- Outcomes: The financial results driven by exceptional patient outcomes.
Let's take pediatric asthma as an example. Air pollution is a major determinant of childhood asthma, but the magnitude of effect is not shared equally across the population, regions and settings where people live and work. Environmental factors that contribute to asthma, in addition to polluted air and water, are often related to economic vulnerabilities such as poverty including the presence of allergens like dust mites and mice, and greater physical deterioration of local buildings. Environmental hazards, especially diesel particulate matter, correlate to pediatric asthma risks, but so do social factors like chronic stress, violence, and separation and instability. Where a neighborhood is faced with both environmental hazards and unmet social needs, the effect is multiplied.
From a cost perspective, hospitals likely will see greater expenses for pediatric asthma in terms of readmission rates and emergency department (ED) utilization. Patients experiencing socioeconomic hardships frequently find it difficult to schedule regular doctor visits — often due to lack of insurance or transportation — meaning they either present with more serious symptoms or rely on the ED for issues that are typically best treated in a primary care setting.
The question then becomes how to increase quality of care for everyone, especially the most vulnerable patients. The first step is identifying the gaps — what is missing from your community that could lead to better health? It's helpful to look at the nine main drivers of social needs:
Once the drivers that most affect your community are identified, providers can start down the long road to ensuring better patient outcomes — including supporting a healthier supply chain and providing local job opportunities and economic growth through programs like Community Contracting.
Where can I find the in-depth data I need to understand my community's needs?
The best tool to explore a community's complex social needs is the free, patent pending Vizient Vulnerability Index™, which allows users to support social drivers of health at the neighborhood level. In addition to drawing from the Vizient Clinical Data Base, the index incorporates numerous external data sources.
Combining public data about neighborhood resources with patient data from more than 1,000 hospitals across the country reveals complex interactions among social needs and health outcomes that may not be clear on a smaller scale. Other indices have a single index algorithm for the whole country, while the Vizient Vulnerability Index adapts to the local relevance of each domain as it correlates to life expectancy. This allows for variation in the weighting of domains across different geographic areas depending on what's important. For example, the most relevant factors affecting health in Lincoln, Nebraska, might not be the most relevant in New York City.
Having an index that works across the country and hospitals serving patients in every state provides a view into the big picture of how all the relevant factors combine in different ways in different places. One hospital or one health system may serve an area where disentangling multiple factors is impossible, but with a nationwide data set we have neighborhoods with poverty and air pollution, neighborhoods with poverty and clean air, and neighborhoods with air pollution but very little poverty. With all the combinations of factors the relationships can become clear.
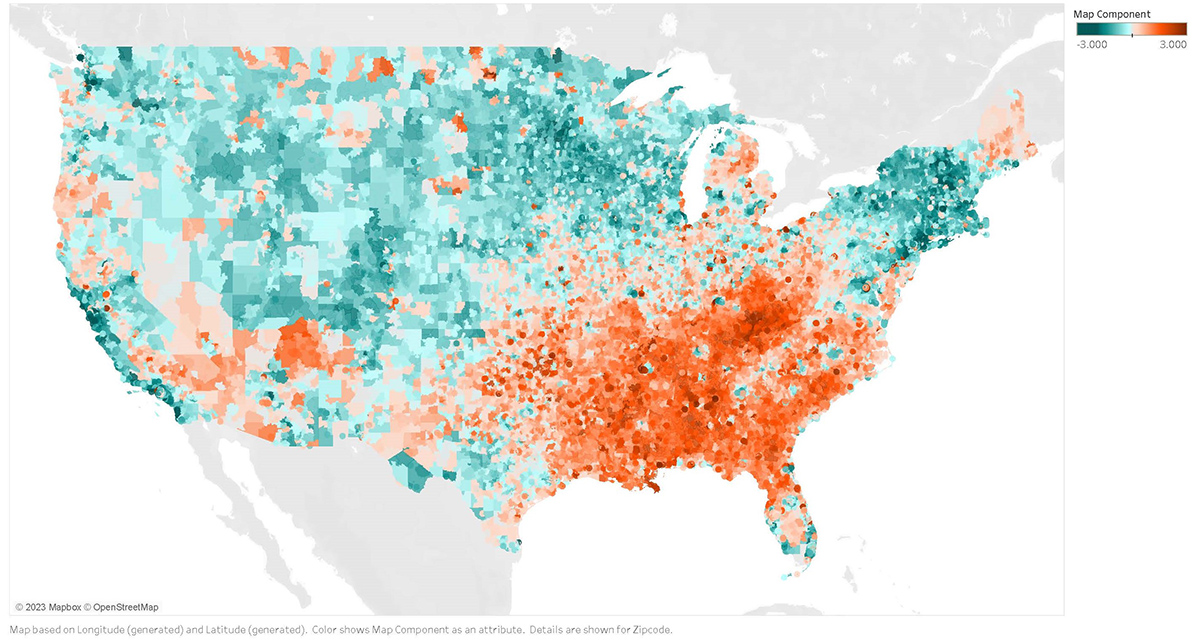
As seen below, nationwide variation in the overall index reflects different combinations of factors in each local area, which is vital for hospitals to understand as they work to better serve local patients.
What are my next steps to reduce risk and improve care?
Collaboration. If the data proves anything, it's that this journey is too substantial for providers to embark on alone — it's one that requires commitment from the entire healthcare ecosystem as well as community organizations and government entities. One particularly helpful resource is the United Nations Sustainable Development Goals, which is a shared blueprint for peace, prosperity, people and the planet.
In terms of CQO, it's crucial to look outside the four walls of the hospital:
- Cost: The investment we make in neighborhood resources contributes as much to disease prevalence as the investment we make directly to healthcare.
- Quality: The care we provide must encompass care for patients in the healthcare setting as well as the care of neighborhoods and the resources provided to our community.
- Outcomes: Building strong communities supports the health of our neighbors and provides the resources people need to maintain their health outside of the hospital.
By delving into the data, we can truly see the interconnectedness of sustainability and health equity so that everyone — from providers and suppliers to local governments and nonprofits — can effectively and efficiently work together to ensure we're living up to the Hippocratic Oath of "First, do no harm."
Learn more about how Vizient is advancing sustainability and health equity across the continuum of care and explore the Vizient Vulnerability Index™.
About the authors
Cristina Indiveri, M.S., is associate vice president of core tenet programs at Vizient. In this role, she guides the strategy of Vizient’s Environmental Sustainability Program while accelerating Vizient’s leadership in sustainability practices across healthcare. She is responsible for collaborating across a wide set of functions to employ solutions and insights to reduce negative human and environmental health impacts while empowering smart, sustainable and resilient choices.
Heather Blonsky is a lead data scientist with Vizient’s Center for Advanced Analytics and Informatics, working closely with providers to develop measures of health equity and patient-centered healthcare quality. She has spoken widely on general health equity topics, as well as on specific issues that became obvious during the outbreak of COVID-19 and how we can apply those lessons to a more actionable approach to health equity.