A truth in health care delivery is patients expect and deserve care to be highly reliable—from both an experience and outcomes perspective. The second truth is the individuals who chose to dedicate their professional careers to “healing” want that too.
Vizient and industry leading high-reliability organization (HRO) company Safe & Reliable Healthcare (S&R) agree and have partnered to advance the application of high reliability in health care. They recently released The Framework for High Reliability Healthcare, a white paper that serves as a next-step blueprint for advancing hospitals’ and health systems’ journey towards high reliability and supporting organizational resets post-COVID.
As health care organizations transition away from a pandemic that tested the very core of their culture, workforce and operations, new perspectives about their strengths and opportunities emerged. Organizations that had prioritized building healthy cultures grounded in collaboration, trust and respect were better prepared to face the crisis with a unified leadership team and workforce. Organizations that had built strong improvement infrastructures grounded in collaborative problem solving, improvement science and transparency had the management systems to stay focused and tackle new challenges that emerged hourly. High reliability embodies building healthy cultures and dependable improvement infrastructures and these are the characteristics that allowed some organizations to emerge with powerful stories to share.
HROs strive for failure-free operations amidst extraordinary levels of complexity and potential error. Examples of high reliability can be found in air traffic controllers, nuclear submarine operators and space flight command centers. The same complexity and risk for harm exists in health care and high reliability as a strategy to decrease patient harm, was elevated by the Institute of Medicine in 1999, in the epic document To Error is Human: Building a Safer Health System. Some may say high reliability in health care is a buzz word and new flavor of the day but the principles that define an HRO are inarguably imperative for providers to deliver to patients (and families) the experience and care they deserve and create a work environment that recruits and retains our very fragile workforce.
Health care HROs acknowledge how easy it is for humans to make mistakes while working in their very complex organizations and delivery systems. HROs mitigate these risks by transforming cultures and designing systems and processes to limit errors by either avoiding them or catching them early so impact can be minimized. More importantly, when the inevitable potential or actual error occurs, they are embraced as a learning and improvement opportunity. Celebrating a near miss, avoidance of potential harm, is as common and important as celebrating the achievement of financial goals.
According to Gena Futral, executive principal, reliability and management systems at Vizient, to achieve health care high reliability there must be an equal focus on the socio (cultural) and technical (management systems) aspects of care delivery. Building healthy cultures grounded in respect, trust, voice and learning is as critical as building infrastructures grounded in improvement science, visual management, transparent data and standard work for all. Once both of these are realized, the shared desire for exceptional experience and outcomes can be consistently and reliably delivered. This creates a healthy and simply, a more enjoyable, environment for the workforce, patients and families; each of these groups have choices about where to work and where to seek care.
“The cultures, systems and processes of HROs are designed to effectively manage the unexpected and mitigate the risk of error—they are continuous learning and improvement organizations,” she says. “Organizations who prioritize high reliability, create an army of problem solvers who are mindful of the risk around them and feel accountable to effectively manage the intricacies of very complex systems. There is alignment around organizational priorities and there is a defined infrastructure for deployment, improvement and sustainability.”
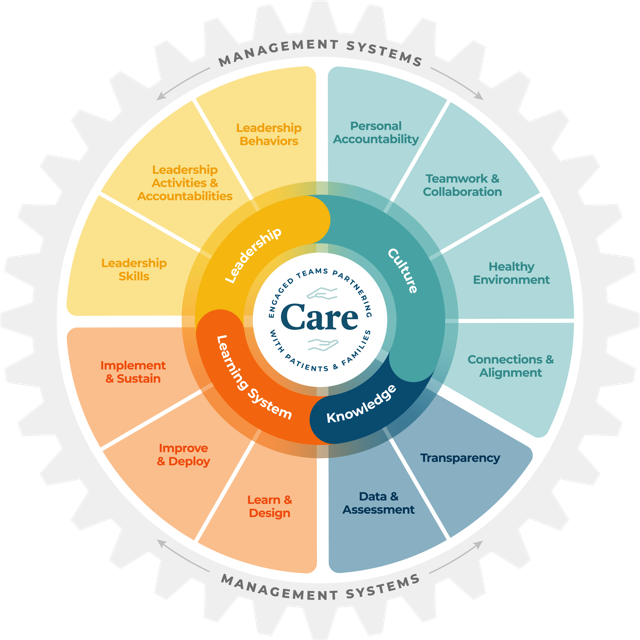
“The framework described in this white paper is designed to capture in one place all the theories, approaches, knowledge sets and activities required for high reliability transformations,” says Amelia Brooks, Safe & Reliable Healthcare, chief knowledge and innovation officer. It’s grounded in five pillars that can guide organizations toward greater reliability, regardless of where they are in their high reliability journeys.
Visually, a gear mechanism is used to illustrate perpetual movement, reflection and continuous improvement and learning, which is the high reliability journey. The pillars are designed for actionable strategies around culture, knowledge, learning and leadership. The pillars connect to an overarching fifth component, management systems which builds the required infrastructure to align and engage executives, middle management and frontline workers around organizational priorities and strategy deployment.

“Cultural transformation is a critical step in achieving reliability, and it starts with leaders adopting a shared definition and language for high reliability and appreciating their essential role in leading cultural transformation. As they align around high reliability principles, leaders can embed the necessary skills, behaviors and activities that create healthy cultures, harness knowledge, drive learning and transform leadership, says Michael Leonard, Safe & Reliable Healthcare CMO. When leaders go first, they can coach the rest of the workforce in high reliability and thoughtfully engage the entire organization around clinical, operational and cultural organizational priorities.”
An important component of high reliability involves appreciating the profound impact culture has on performance. Once this is accepted, having valid tools to measure culture, clinical and operational performance is essential. It is not enough to analyze these disparate data sets independently, integrating this data creates new insights into performance drivers. Futral notes that identifying the cultural factors as the root cause for opportunities is not a routine approach in health care performance improvement. Through this innovative way to integrate data, organizations gain new insights into where they are, where they want to go and the explicit actions necessary to advance; all are important contributors to developing an individualized roadmap.
Though high reliability emerged from the safety movement, all performance imperatives can be tackled by applying the framework. High reliability creates healthy cultures and that in and of itself, improves the daily experience of the workforce. If the workforce is having a better day, patients and families benefit. Management systems create the infrastructure, competencies and capabilities to improve and sustain performance from the bedside to supply chain. High reliability is an important strategy to achieve and sustain clinical, operational and cultural performance excellence across the entire system of care.
Support for hospitals creating HROs
Vizient’s HRO solution is a comprehensive high reliability solution and includes expertise grounded in high-reliability principles, management systems, technology and analytics. The partnership with Safe & Reliable brings decades of experience to serve as partners for organizations aspiring to embed high reliability into their organization. The partnership elevates the analytical capabilities of both companies and creates new insights through the integration of Vizient’s robust clinical and operational data with Safe & Reliable’s culture of safety, burnout, resiliency and engagement data.
This solution can support organizations regardless of where they are on the high reliability journey. Assessing and measuring current clinical, operational and cultural current state may be the place to start and with these insights, develop a transformative and comprehensive high reliability roadmap that defines where to focus to improve specific metrics. Perhaps, clinical, operational or cultural measurement is needed to understand current state. We can start more focused to educate and align leaders on their roles and actions they can take immediately to start cultural transformation without ever engaging the workforce. Another initial strategy could be to assess the maturity of existing managements systems and identify opportunities to increase the effective deployment of improvement imperatives across the organization and decrease variation.
Each organization is at a different place, the important first step is embracing high reliability as an important strategy to re-set your organization post-COVID, re-engage your workforce and re-align and re-deploy organizational clinical, operational and cultural improvement imperatives. You may not even call it high reliability though you have goals to achieve and sustain performance excellence and appreciate the need to equally focus on culture and improvement infrastructure. It is not important what you call it, the important first step is understanding where you are, developing a comprehensive plan and getting started.
