by Annette Alexander, Kate Lizzi and Kristi Blitz
Clinical Advisory Solutions
This blog post is part two of a five-part series on clinical-supply integration, a process for informed business decisions that engage clinicians, preserve quality and safety and lead to greater patient satisfaction. Read the other blogs in this series:
- Transitioning from Value Analysis to Clinical-Supply Integration: It’s All About the Process
- Moving from Value Analysis to a Clinical-Supply Integration Model: Engagement and Alignment are Key
- How Do You Know What You Know? 3 Ways Clinical-Supply Integration Can Help You Make Better Decisions
- Clinical-Supply Integration vs. Value Analysis: Is There a Difference?
As John D. Rockefeller once said, “Don’t be afraid to give up the good to go for the great.” It’s hard to argue with Rockefeller’s successful approach to business. To apply his philosophy in supply chain, we need to rethink our approach to product decision-making.
Success in the evolving health care market requires an ongoing, interdisciplinary partnership between clinicians and supply chain professionals to understand the differences in products that may affect quality outcomes and cost. While standardizing clinician product choices is a good start, we need to move toward clinical-supply integration (CSI), a collaborative decision-making platform led by physicians.
Using data to improve total cost, quality and financial outcomes
As organizations tap physicians to lead the charge in CSI, they must provide them with comparisons of cost, utilization, clinical variation and benchmarking. To do so, organizations need to leverage actionable, integrated supply, clinical and operational data.
Supply Data
- No direct link between supply data and electronic health records
- Demonstrates changes in purchase volumes and line item pricing, and savings impacts based on those trends
Clinical Data
- Identifies differences in physician practices and patient populations
- Found in the electronic health records
- Includes patient length of stay
Operational Data
- Shows supplies used and the pathway of care of a patient encounter
- Includes subset of the patient encounter data, found in the electronic health record
- Outlines the difference in patient types and procedural settings
When integrating these data sets, two key steps must take place. First, ensure the final data set is actionable. Second, confirm that the method to compile and update the data is sustainable.
Once your integrated data set is compiled, two primary methodologies can be used to move patient outcomes from good to great: the development of category management and the identification of practice variation. Let’s take a deeper look at each of these to better understand how CSI uses data differently than a traditional product standardization approach.
Category Management
Category management is a strategic approach that identifies and reduces unwarranted variation in cost and quality. This strategy aligns and engages organizations into specific groups of supply and/or service categories.
The data used within category management includes market insights, national benchmarking and patient outcomes.
The benefits of implementing category management include:
- Engaging cross-functional category management teams, including clinicians, supply chain sourcing, contracting and value analysis
- Giving equal weight to strategy, internal and external benchmarking, clinical acceptance, and cost and quality impact
- Defining your organization’s guiding principles that lead to optimized contract value, clear objectives and actionable data all working together to create a continuous lifecycle of improvement.
|
Good: Traditional Approach |
Great: CSI Category Management |
|
Limited Collaboration
|
Expanded support with enhanced clinical input
|
|
Single Focus
|
Expanded Focus / Process
|
|
Supplier Interaction
|
Supplier Engagement
|
Practice Variation
Practice variation connects data from supply, clinical and operational databases to identify overall clinical practice variations in cost and care. In order to execute at a CSI level, we combine the data from these three sources to make informed decisions about patient care.
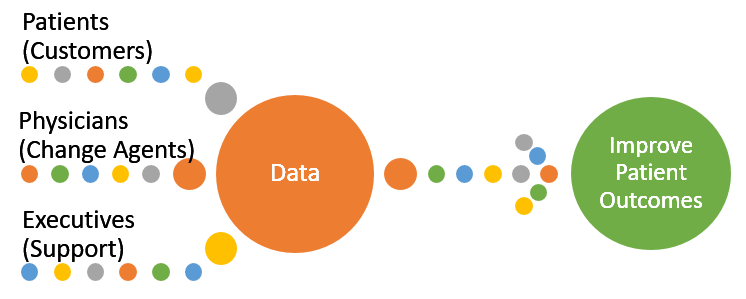
The overall goal in a CSI model is an improvement in patient outcomes through a reduction in practice and product variation. Variations become the center of physician peer-to-peer conversations. The patient is the customer, the physicians own and drive the change, the executives support the determinations and the data is the epicenter providing direction.
The benefits of identifying practice variation include:
- Standardizing care, better clinical outcomes, increased revenue, supply cost reduction and consolidation of like products
- Peer-to-peer discussions using actionable data to promote variation reduction
- Positive impact on outcomes measurements including length of stay, readmissions, mortality and complications
|
Good: Traditional Approach |
Great: CSI Clinical Practice Variation |
|
Supply chain data
|
Determining cost/case variation
|
|
Clinical data
|
Physician specific practice variation
|
|
Operational data
|
Physician-specific operational variation
|
What are the next steps in moving toward a CSI data driven model?
The starting point is to engage with the clinical stakeholders, ideally at the service line level. Know your facts and validate all data before engaging your physicians. Once you know their total cost of care and how that cost compares to others, you can build an actionable plan. Listen to the needs and concerns of your physician partners. Physicians’ professional goals must also be considered so that all parties can find common ground. This will build their trust to engage in the CSI process and, more importantly, motivate them to lead the process.
Next, executives must understand and acknowledge the necessity and benefits of physician leadership, expertise and participation in clinical and cost management efforts. Together, clinicians and executives will drive the CSI message across the organization. Recognize that opportunities for improvement may lie in multiple areas, including contracting, physician product selection, overall clinical practice and revised plans of care.
With actionable data and strong physician leadership, your approach to supply decision-making will soon move from good to great.
Clinical-supply integration is an ongoing, interdisciplinary strategy encompassing four performance domains — engagement, insights, process and knowledge — to inform decision making about products and services in order to eliminate harm, improve outcomes and lower costs. Read about the domains in the related articles below or learn more about clinical-supply integration.
About the authors