By Erin Cristales
Vizient
“Without entities like Vizient that are adding disability to their equity data and can help us define, and more importantly measure, the efficacy of interventions, we’re never going to be able to drive that culture change.” — Dr. Wendy Ross, Director, Jefferson Health’s Center for Autism and Neurodiversity
I hope I did something wrong.
It was Heather Blonsky’s first thought when she saw the results.
Anecdotally it seemed obvious that populations with intellectual disabilities were more likely to fall victim to COVID-19, but the exact risk had not yet been quantified — and certainly not with the confidence afforded by Vizient's Clinical Data Base.
That's why in January 2021, Dr. Jonathan Gleason reached out to Blonsky, Vizient lead data scientist. The two served together on Vizient's Health Equity Steering Committee, and in discussing the perils faced by frontline workers, they began to contemplate a separate, if related, question: What about other people who couldn't completely isolate — and, in many cases, were unable to follow common behavioral interventions such as ► mask wearing and social distancing?
It was a problem that had plagued Gleason since the early days of the pandemic when he served as chief clinical officer and EVP of Jefferson Health in Philadelphia. He saw firsthand the devastating impacts of the virus at long-term care facilities that housed patients with intellectual disabilities. At one point, the toll was so brutal that the National Guard was mobilized to help handle the outbreak.
So, he asked Blonsky to tap into the Clinical Data Base's incomparable breadth of data to better appraise the risks faced by an already vulnerable population. Using the CDB, she created a cross-sectional study of 64,858,460 patients across 547 healthcare organizations. Of those patients, 128,074 were documented as having intellectual disabilities.
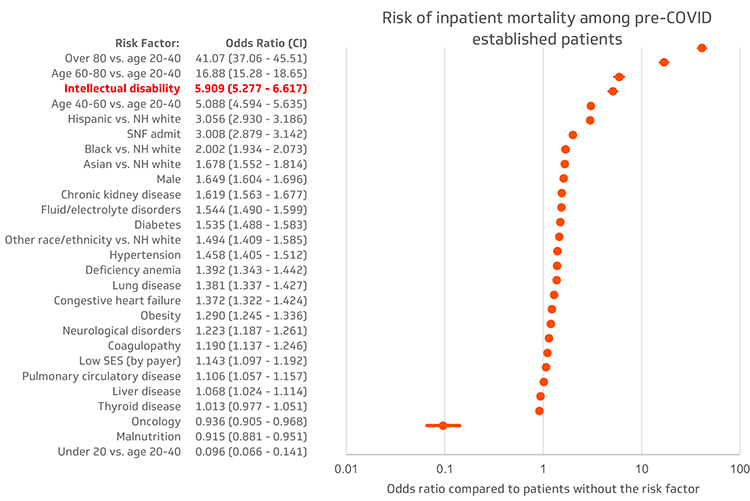
What Blonsky found, though not entirely unexpected, was nonetheless startling in its severity: The data showed that having an intellectual disability was the strongest independent risk factor for a COVID-19 diagnosis. It also revealed that the adjusted odds ratio for those patients dying from the virus was a whopping 5.9 — making intellectual disability the most significant independent risk factor other than age for COVID-19 mortality.
But in those findings emerged an unexpected silver lining. The direness of the data would ultimately serve as an urgent wakeup call — one that would rouse governments across the globe to, at long last, act.
'Data drives the policy'
On March 5, 2021, Blonsky and Gleason — along with Dr. Wendy Ross, director, and Alexander Fossi, research coordinator, at Jefferson Health's Center for Autism and Neurodiversity, and Dr. Mary Stephens and Jane Tobias, assistant professors at Jefferson Health — published their findings in a New England Journal of Medicine Catalyst article titled "The Devastating Impact of COVID-19 on Individuals with Intellectual Disabilities in the United States."
The Pfizer and Moderna COVID-19 vaccines had received emergency use authorization by the FDA three months before, with the Janssen vaccine following in February. Prioritization protocols from the Centers for Disease Control included the elderly, immunocompromised, and those living with comorbidities such as diabetes, obesity and heart disease.
Absent from the list: People with intellectual disabilities.
Blonsky, Gleason and Ross knew that needed to change. They had undeniable evidence that COVID-19 posed an astronomical risk to those with ID — not just in terms of contraction and overall mortality, but also in elevated rates of hospital admission and ICU stays.
But would the data resonate?
Five days after the study's publication, civil rights lawsuits were filed in states across the country by families of individuals with intellectual disabilities demanding prioritization for their loved ones. The Special Olympics issued a press release about the study that quoted Gleason and Ross. On March 11, Ross published an op/ed in the Philadelphia Inquirer detailing the "unconscious and conscious bias that has long infiltrated medicine." Both healthcare and society need to reframe perspectives on what makes a life worth living, and how we support each other to reach our potential, she wrote. ► Helping those more vulnerable ultimately helps us all.
"It's fair to say we got a little noisy," said Gleason, now chief clinical officer and executive vice president of Prisma Health.
On March 19, Kentucky and Philadelphia (which cited the study in its decision) expanded their phase 1B qualifications for the COVID-19 vaccine to include those with intellectual disabilities. That same day, the momentum reached global proportions when Japan's Ministry of Health, Labor and Welfare also added intellectual disabilities to its prioritization list. Other countries, including India, soon followed.
"Math has a way of spotlighting issues clearly and undeniably," said Blonsky, who has nearly 30 years of experience in examining health equity data, including with the new Vizient Vulnerability Index™.
There was certainly strength in the numbers, Gleason agreed — and the results "wouldn't have been possible without the sheer expanse of the Clinical Data Base."
"What can we do with that scale of data?" he asked. "In this example, in just a couple of weeks, we were able to change a lot of things about the world."
And those changes just kept coming. In late March and early April, Delaware and New Jersey also added intellectual disabilities to their vaccine priority lists, with other states eventually expanding prioritization as well. Then, in February 2022, the holy grail: The CDC added intellectual and developmental disabilities to its list of high-risk conditions.
"The data drives the policy," Ross said. "And the policy creates the practice."
From left, Heather Blonsky, Dr. Wendy Ross and Dr. Jonathan Gleason present at the 2022 Vizient Connections Summit in September.
'Good trouble' leads to more solutions
Less than 24 hours before they joined Blonsky to present the results of their study to providers at the 2022 Vizient Connections Summit in late September, Gleason and Ross found themselves in a small conference room in New York City. Inside were U.S. Surgeon General Vivek Murthy, Deputy Director-General of the World Health Organization Zsuzsanna Jakab, and Tim Shriver, Chairman of the Board of Special Olympics International. The crux of the discussion was how to make healthcare more equitable and inclusive for those with intellectual disabilities, and Gleason and Ross were buoyed by the future-focused nature of the conversation.
While the March 2021 study had made an undeniable splash and a noticeable difference with the extension of ► vaccine access, it was only the first of many dominoes that needed toppling. The team knew this was no time to dust off their hands and declare mission accomplished.
"We created good trouble," Gleason said. "We need to work on creating more awareness and more solutions."
While vaccine prioritization was a step in the right direction, there were still ► concerning gaps in care and misperceptions about patients with intellectual disabilities. A study published in the February 2021 issue of Health Affairs found that more than 80% of U.S. physicians reported that people with significant disabilities have worse quality of life than nondisabled people — an attitude that may contribute to healthcare disparities and "is not an opinion that people with disabilities share," Ross said.
In October 2022, JAMA published research outlining three major systemic health inequities for individuals with intellectual and developmental disabilities, including stigma, exclusion and devaluing the equal worth of persons with IDDs; underrepresentation in population epidemiology and research; and inadequate access to high-quality care and social services tailored to needs. A few days later, The New York Times printed an article headlined, "These Doctors Admit They Don't Want Patients With Disabilities."
"There is a lot of work to be done," Ross said. "Without entities like Vizient that are adding disability to their equity data and can help us define, and more importantly measure, the efficacy of interventions, we're never going to be able to drive that culture change."
Prior to the March 2021 study, Ross had never worked with Blonsky, Vizient or the Clinical Data Base. Now, she's a member of Vizient's Health Equity Steering Committee and has recruited Blonsky for additional research projects that draw on information from the CDB (which now contains data from more than 1,000 healthcare facilities). One of those projects involves looking at colorectal and breast cancer care for patients with intellectual disabilities, particularly related to preventative measures such as screenings. The goal is to determine if there is a lack of equity in terms of preventative care that leads to patients with intellectual disabilities presenting with more progressive forms of cancer.
The key, Blonsky said, is for providers to keep asking questions that can ultimately lead to solutions. The data is there. It's just a matter of surfacing it.
"► Equity is a lot of different things — with intellectual disabilities, we have another piece of the puzzle that brings more nuance, more accuracy and more of what we need to make healthcare inclusive," Blonsky said. “I always want to dig in more. The part of my job that I love the most is when we come together and say, 'We've done the math — now what are we going to do about it?'"
Learn more about how Vizient is advancing health equity.