Health care organizations have long understood the opportunities inherent in working together to develop solutions that address individual challenges. Powered by automated data collection and analysis tools not available 10 years ago, aggregation groups are evolving their focus to include both buying and usage behaviors to maximize supply value.
As a pioneer in the concept of aggregation groups, Vizient works hand in hand with members to meet them where they are when it comes to aggregation strategies.
“While price is a major driver in aggregation, the days of exclusively focusing on price are long gone,” said David Gillan, senior vice president, member business ventures at Vizient. “Health care organizations are coming together around value beyond supply cost collaboration. The groups we work with are closely evaluating the benefits of product standardization, utilization strategies, care delivery process improvement, outcomes-based supplier contracting, and new ventures to realize cost savings and revenue opportunities for their organizations.”
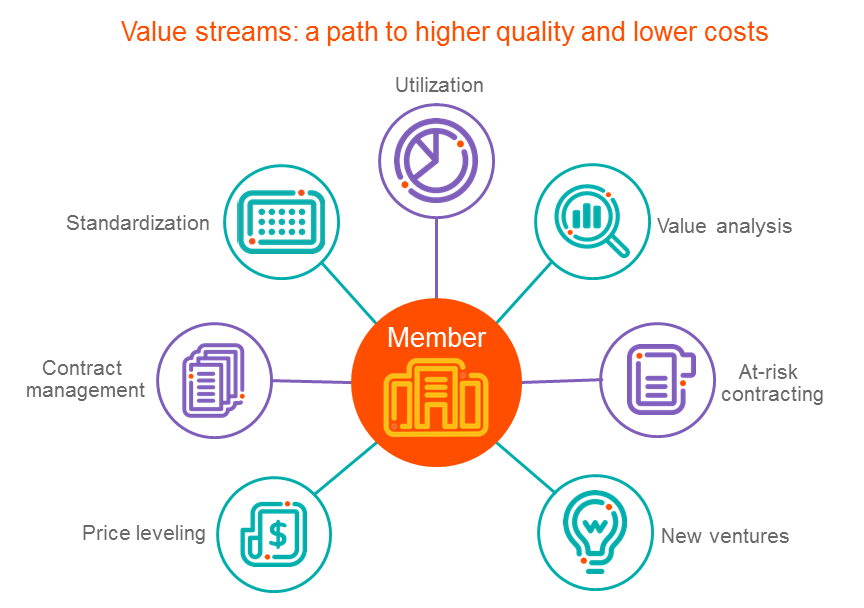
Vizient has identified seven value streams that serve as pathways for member aggregation groups. While the value streams build upon one another, groups may find themselves in more than one stream as they address different product and spend categories.
Price leveling
In this value stream, groups leverage price transparency to reduce cost variation of supplies. Price leveling requires members agree to certain compliance requirements or behaviors to achieve better pricing. This often comes in the form of information sharing for the purpose of tracking and improving organizational compliance.
Compliance monitoring is a fairly new element of price leveling that has come from new data and analytics tools and it is a game-changer. “If a group says they are going to be 70 percent compliant to a category to get that better price, it’s no longer just their word, it’s their data. It keeps all parties engaged in compliance,” said Gillan.
Contract management
In this value stream, groups are focusing on validating the application of negotiated supply pricing, using preferred vendors, enforcing adherence to terms and conditions, and validating receipt of discounts or rebates.
A simple example of contract management is the use of products that are inside and outside of NOVAPLUS®. If a product is not flagged properly in a hospital’s MMIS system, they’re not getting the NOVAPLUS price, they’re getting the national contract price for the branded product. While that is still a savings, it’s not the lower NOVAPLUS price.
Standardization
In the standardization value stream, the members of the aggregation group are evaluating clinical products, equipment and technologies, and developing supply management policies for item selection, ordering, distribution and disposal. This work can meet with resistance from clinicians, so evidence and education is essential to success. Clinicians can still be offered a level of choice and functionality while reducing variation to increase efficiency, enhance safety and save organizations money.
“Standardization is critical but oftentimes misunderstood. We recently worked with one group that went from 18 SKUs for gloves to three. This reduction in item count creates a significant cost savings to the member and improved operational efficiencies because they don’t have to stock, pick, pack and deliver 18 gloves to multiple facilities. That creates efficiencies and fuels a strategic member-supplier partnership where there are economies for both sides,” said Gillan.
Utilization
Managing the utilization of supplies includes equipping clinicians with product and pricing information needed to optimally use supplies and manage the total cost of care, as well as an understanding of the outcomes of their adherence. In many cases, organizations encourage suppliers to do in-service education with individuals using their products to ensure they are applying and using them properly. For example, understanding red-bag waste – what goes in versus what does not – could save hospitals $10-$12 million per year.
Value analysis
In the value analysis value stream, supply chain leaders and clinicians are working together to understand the clinical efficacy of a product. This work involves the application of defined, unbiased processes with stakeholders across the aggregation group for the selection of medical devices and other preferred products. Value analysis is often best undertaken with the help of nurses, who are influential across all value streams and responsible for meeting with supply reps, managing supply usage and tracking product changes.
According to Gillan, this is where many hospitals have savings leakage. “An analogy for the issue is when you buy a car. You negotiate and agree on the price and then they ask if you want heated seats. Those are an upgrade so the cost goes up. In health care, upgrades are usually locally negotiated add-ons which create savings leakage. But if a group is linked with a GPO for value analysis, and strategically engaged with a supplier, we’re going to curtail the amount of upgrades and leakage.”
At-risk contracting
This value stream requires strong and strategic relationships between suppliers and members. Both parties freely share data and value based on clinical outcomes associated with specific medical devices. In “at-risk” scenarios, suppliers believe so strongly in their products and their customers’ abilities to manage their contracts, standardization and utilization, that they accept payment based on outcomes, or “at risk.” At-risk contracting can lead to improved efficiencies, better outcomes and mutual cost savings for both organizations and suppliers.
“At-risk contracting is not for the faint of heart,” notes Gillan. “Not all suppliers are going to do this and you don’t want to do this with all suppliers. Vizient helps members identify and engage with suppliers for at-risk contracting initiatives. They don’t have to be biggest companies, but they have to be very engaged.”
New ventures
Aggregation at its most sophisticated can be seen in the new ventures – nontraditional businesses, partnerships and cost-savings models – developed by participating hospitals and health systems. Ventures may be as simple as co-ops around laundry or food facilities, or as complex as clinical pathways that may be offered to other organizations as blueprints for clinical care.
Vizient’s seven value streams offer a path to better quality care and lower costs, but individual organizations often begin from very different points along the continuum. It is important for each organization to consider its respective goals, culture and organizational readiness as they assess how they ladder up to the activities and resources of a given aggregation group.
“We recognize our members have varying levels of experience and interest related to each of these value streams, and that we need to help them evaluate where they are and what approaches are best for their organizations,” Gillian said. “As we look to the future, we are developing tools that will help to inform these conversations. These tools will never replace personal, strategic consultation, but they can help us establish a baseline and track, measure, and monitor our progress.”
For more information about Vizient’s aggregation services, contact Kevin Galyean, director, member business ventures.