By Sherri Mason, , MSN, BSN, APRN, FNP-C
Vizient Consulting Director, Advisory Solutions
Financial challenges continue to mount for health systems. Dozens of hospitals announced layoffs during the first quarter of 2023, and some are closing entire facilities. According to Municipal Market Analytics, eight hospitals defaulted during Q1, including some large, highly rated systems — the most since 2011.
With little relief in sight, it is critical that health systems drive new efficiencies to increase revenue and cost savings. This is especially true for the operating room, which represents both the largest revenue driver for health systems and the biggest cost center. According to Definitive Healthcare, the 20 hospitals with the largest spend on OR supplies totaled $5.5 billion in operating room costs. The average total operating room costs for these hospitals was $274.5 million.
Improving efficiencies in the OR can add millions to a health system's bottom line. Scheduling cases can be as much an art as a mathematical science so when there is a change to the timing of one procedure, whether prolonged due to an unexpected patient event or avoidable due to inefficiencies, the cadence of the day is impacted and can result in canceled cases that may affect operating costs, staffing, revenue, and potentially patient outcomes. Leading health systems that operate highly efficient surgical programs generate greater procedure volumes and profits while reducing supply costs. Physician and staff satisfaction from a more efficient department may also help to limit turnover, which can be a significant cost savings.
Vizient is seeing increased provider interest in optimizing preference cards, given the financial pressures that health systems are experiencing. Preference card work has been sidelined in the past due to complexity, but as organizations realize that they have addressed the majority of "low-hanging fruit" opportunities, there is an increased awareness of the untapped savings available by improving efficiencies — and preference cards play a major role in that efficiency within surgical departments. Surgical leaders and staff know preference cards are inaccurate but do not always know where to start the process to improve them, which is why assistance is sometimes required from outside the organization to achieve a sustainable preference card management program. I sometimes compare it to untangling a ball of yarn — it's hard to know where to find the end.
Pursuing physician preference card optimization as a strategy to uncover hidden savings
Preference cards inform clinical staff of the supplies needed so surgeons have the right supplies for the right patient at the right time for the right case. Accurate preference cards minimize waste, both in materials and spending, and increase charge capture leading to revenue opportunities.
Typically, savings from preference card optimization can be measured as early as 60 days, although more substantive results can take longer to reflect the accurate card's impact on supply chain ordering. Regardless, savings can be significant:
- By working with Vizient to optimize its surgical preference cards database, the University of Washington health system saved more than $1 million.
- Intermountain Healthcare reduced the number of cards it uses by more than 50% to approximately 22,000. By doing so, the IDN's Surgical Services Clinical Program team reduced costs for unnecessary supplies by more than $2.5 million.
When a project begins, we find that the majority of preference cards are inaccurate, not because health systems are unaware of the importance of maintaining them, but because they have lacked the capacity to tackle the job for so long and for a multitude of valid reasons. With staffing shortages, staff and surgeon turnover, supplier changes, backorders, and so many other time conflicts, it's an administrative task that gets relegated to last position even though it may have a direct impact on patient safety, patient care, supply utilization and department satisfaction scores.
Accurate preference cards are as critical to patient safety as they are to OR efficiencies
In many of Vizient's project surveys, surgeons respond that their cards are inaccurate, which may require operating staff to leave the room during the procedure to locate missing supplies. This could translate into increased anesthesia time and less attention to the patient. As these delays continue from one case to another, there could also be prolonged case times requiring staff overtime.
Charge documentation may also be impacted by incorrect preference cards due to the time it takes to find and add missing items or decrement items not needed to the record during the procedure. More concise and accurate cards will contribute to better inventory management and fewer errors in procedure charges. This also results in a reduced number of supply returns — supplies not needed or not charged for impact PAR levels and consume valuable staff time for restocking and resupplying. Unshelved returned products are also "invisible" to inventory management and may be creating discrepancies that result in outages or unneeded surplus. For those unneeded products that are opened and discarded, the waste is not just the cost of the products discarded but also increasing costs for managing the waste created.
This is especially impactful considering that many health systems rely heavily on temporary labor staff that carry wages nearly twice that of staff nurses. With some hospitals nearly 60% reliant on travel nurses for staffing, optimized preference cards can help travelers be more efficient in their daily routines, as opposed to in-house staff that possess high amounts of "tribal knowledge." Rote behaviors may also contribute to erroneous setup when the preference cards aren't trusted as the source of truth, as setting up cases from memory may not bring awareness of recent backorders or supplier product changes.
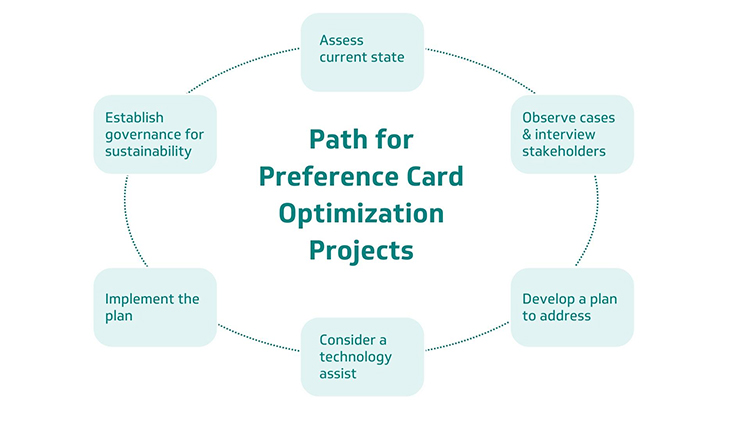
Inaccurate preference cards don't just impact the OR. Workflows and processes beyond the operating suites are impacted throughout the hospital supply chain, from scheduling to sterile processing and materials management to restocking and ordering. The below graphic depicts a basic project path for preference card optimization projects, starting with assessing the current state within the health system.
Considerations for updating preference cards
When undertaking a program to update preference cards, it's important to remember the following:
- It is crucial to optimize preference cards. Many providers say that prior attempts resulted only in reducing the spend associated with the overall card cost, which actually creates a more inefficient process once a procedure begins and products are missing. Paring down preference cards to the bare minimum does not equate to optimizing them.
- Nurses and OR staff may not be immediately aware of supply backorder or commodity changes. Staff may set up a case without referring to the cards, usually because they don't trust them. Creating accurate cards and restoring trust in the document can avoid waste and improve efficiency in the OR.
- When inaccurate or obsolete cards exist, case schedulers have difficulty locating and selecting the appropriate card to schedule a case. This can result in the need for a case cart to be rebuilt, delaying a procedure or perhaps even canceling it, which leads to patient dissatisfaction and unnecessary preoperative rework expenses (i.e., labs, transportation, hotel stay, etc.).
Intuitively, it is easy to equate accurate preference cards with a tangential benefit of improving outcomes and length of stay even though we do not yet have a way to provide a direct measurement for confirmation. However, we do know that accurate preference cards reduce waste and supply costs, improve patient safety and operating room efficiencies, and further support better surgeon and staff satisfaction. The key is to clearly assess the current state, devise and implement a clear plan, and sustain those improvements through ongoing governance and internal tracking.
Learn how through expertise, insights and automation, Vizient can help providers deliver customized value in clinical and physician preference item service lines like cardiovascular, orthopedics, spine and neuroscience.
Connect with an expert about your preference card needs.
About the author
Sherri Mason, MSN, BSN, APRN, FNP-C, is a Vizient consulting director with more than 30 years of experience in the healthcare industry. Her professional skills include expert clinical practice, broad knowledge of both clinical and research practices, and clinical and healthcare business leadership. Prior to joining Vizient, Mason spent her career in prehospital care, critical care, cardiac cath lab, interventional radiology and emergency department practice. She is an advanced practice nurse and certified family nurse practitioner and a member of the American Association of Nurse Practitioners. Mason earned a bachelor's degree in nursing from the University of New Mexico and a master's degree in nursing from the University of Cincinnati.