by Keely Macmillan
Vizient Associate Principal, Sg2 Consulting
It’s that time of year! CMS recently finalized a set of changes to the country’s largest alternative payment model (APM): the Medicare Shared Savings Program (MSSP). With a goal of attracting new entrants, retaining existing accountable care organizations (ACOs) and encouraging ACOs with expiring participation agreements to renew their commitment, this broad set of changes constitutes the largest program reform since the Pathways to Success overhaul was finalized in 2018. In isolation, these changes will have varying effects on a given ACO. Now, provider organizations must consider what’s changed—and more importantly, what hasn’t—when refreshing their value-based care (VBC) strategies.
Overarching changes applicable to all ACOs
Among the most significant updates made to MSSP are a series of modifications to the financial benchmarking methodology, as shown below. These modifications will be applicable for agreements beginning 2024 or later and intend to address concerns about the impact of an ACO’s regional penetration and prior cost savings on its financial target.
Accountable Care Prospective Trend (ACPT)
- When updating an ACO’s benchmark, CMS will incorporate the ACPT into a three-way blend with the national and regional growth rates. The ACPT is a prospectively set administrative growth factor and a variant of the United States Per Capita Cost (USPCC).
- Incorporation of the ACPT is an intermediate step towards administrative benchmarks, i.e., tying financial targets to an external index instead of observed spending, and could have a positive, negative, or neutral impact at the individual ACO level.
Changes to Regional Adjustment
- CMS will limit the cap of the negative regional adjustment and further decrease the negative regional adjustment based on an ACO’s proportion of dually eligible beneficiaries and/or the weight of its Hierarchical Condition Category (HCC) risk score change that will have a positive to neutral impact at the ACO level
Amended Risk Score Cap
- CMS is amending its application of the annual adjustment for changes in severity and case mix within an ACO’s attributed patient population.
- Instead of applying a 3% cap for each Medicare enrollment type, CMS will apply a single aggregate risk score cap across enrollment types allowing for a higher benchmark for ACOs treating more complex, high-cost patients.
Other program changes afford ACOs more opportunity to earn savings, such as a health equity adjustment that will alter an ACO’s Merit-based Incentive Payment System (MIPS) quality performance score by 0 to 10 bonus points under certain conditions. CMS also finalized an alternative quality performance standard that allows certain ACOs to share in savings even if they do not meet the minimum savings rate. Finally, CMS confirmed a series of changes aimed to ease the administrative burden of participation.
Program changes most relevant to new entrants
Of significance, for certain ACOs new to MSSP, CMS is providing access to up-front capital, or Advance Investment Payments (AIPs), to invest in the infrastructure necessary to manage care for their population of patients. Eligible ACOs can apply for a one-time fixed payment of $250,000 and quarterly, per beneficiary payments for the first two years of their agreement period. AIPs would not be recouped if the ACO did not earn savings and may attract ACOs treating patients in rural and underserved areas.
In addition, newly entering ACOs without experience in taking on risk will be able to remain in an upside-only track for the duration of their five-year agreement period. These ACOs could remain in upside-only for two additional years of their subsequent agreement period for a total of seven years of experience before gradually taking on downside risk.
CMS also finalized its proposal to make the ENHANCED Track—the track with the greatest level of downside financial risk—optional for all ACOs.
The ability for these ACOs to 1) access capital, 2) remain in an upside-only risk arrangement for seven years and 3) opt out of the ENHANCED track altogether could provide the financial resources and flexibility to succeed in the program on their own rather than turning to an ACO enablement company (an organization that offers downside risk protection and infrastructure support in exchange for a share of an ACO’s savings payments).
Program changes most relevant to participants in upside-only risk tracks
Only 41% of MSSP’s current participants are in upside-only risk tracks; a vast majority of these ACOs would have been required to move to downside risk in 2023. However, CMS has finalized a program change allowing them to remain in their upside-only arrangement for the remainder of their agreement period. CMS also finalized a program change that would allow renewing ACOs that had previously been in upside-only arrangements to start their next agreement period in an upside-only risk track before transitioning to two-sided risk. Coupled with the pending expiration of the advanced APM bonus under the Medicare Access and CHIP Reauthorization Act (MACRA) Quality Payment Program—a significant incentive to move to the BASIC Track E or ENHANCED downside risk tracks—many organizations are expected to take advantage of this new flexibility.
Program changes most relevant to participants in two-sided risk
Currently, a majority (59%) of MSSP ACOs are in two-sided risk tracks; most of these ACOs are in BASIC Track E or ENHANCED and qualify as advanced APM participants. This cohort of MSSP participants, which largely represents the most experienced ACOs, received the fewest number of new flexibilities specific to their participation status.
When renewing their participation agreement, this cohort in particular will benefit from CMS’s new policy of applying an adjustment for prior savings to address the “rachet” effect of an ACO’s past success leading to lower benchmarks. CMS also finalized a modification to the shared loss calculation for ENHANCED track ACOs. While this modification provides some insulation from extreme losses, it’s unlikely to provide meaningful protection given strong performance among most ENHANCED ACOs.
Some experienced ACOs may have already opted to migrate to ACO REACH for 2023 and beyond, and ACOs that remain in MSSP will need to look beyond opportunities or disadvantages presented in CMS rulemaking to remain well positioned amid significant market forces and disruptor presence.
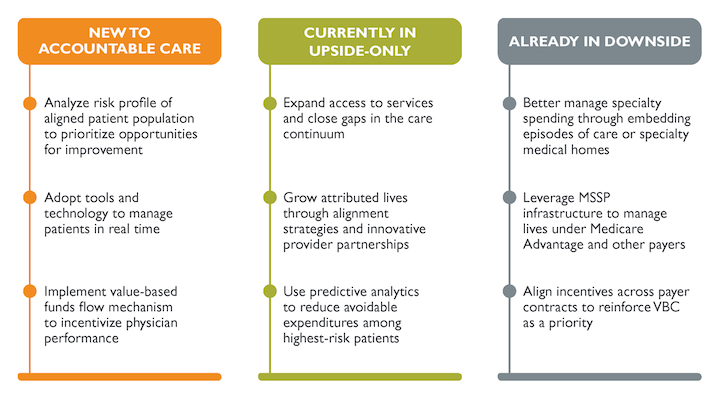
Key considerations by participant group
Regardless of whether your organization is new to MSSP, is still in an upside-only risk track, or is part of the majority of participants that have already moved to downside risk, there is a path forward, with key strategies to support your success.
Learn more about alternative payment models such as MSSP.
About the author
Keely Macmillan leads engagements that assist healthcare organizations transition to value-based payment and delivery models. Drawing on deep payment policy expertise, she partners with provider organizations to identify and implement strategies for success in alternative payment models (APMs) including shared savings arrangements, capitation and episodic payments.