by Shaifali Ray, MHA, Vizient Senior Networks Director
Karyl Kopaskie, PhD, Sg2 Associate Principal, Intelligence
It was about a year ago when the first surge of COVID-19 cases began to ripple across the United States. No strangers to addressing the evolving needs of communities, hospitals and health systems paused elective procedures, provided care to patients and doubled down on efforts to educate their communities about how to slow the spread of the virus.
We have seen how significant the effects of COVID have been on our country’s most vulnerable populations, amplifying existing health disparities. The data is clear about the disproportionate impact of COVID on racial and ethnic minority groups in terms of who gets the virus, who gets very sick and who is dying. We also have seen the disproportionate economic impact of COVID, creating more significant gaps in things like unemployment, resulting in increased food insecurity and homelessness.
As the nation cycled through several more COVID surges, we’ve watched hospitals and health systems continue and expand their efforts to address social determinants of health. This work has taken on new meaning during the pandemic and will continue to become even more important across our nation’s complex landscape of unmet social needs and health disparities.
COVID-19’s impact on disparities
The Centers for Disease Control and Prevention COVID-19-Associated Hospitalization Surveillance Network estimates that compared to Whites and non-Hispanic persons, Blacks are three-and-a-half times more likely to be hospitalized for COVID and almost three times more likely to die from it; and Hispanics are four times more likely to be hospitalized than Whites. The Vizient Clinical Data Base analytics platform—which captures patient outcomes data from our member organizations—is finding similar trends. Our analytics team went one step further and found an interesting insight.
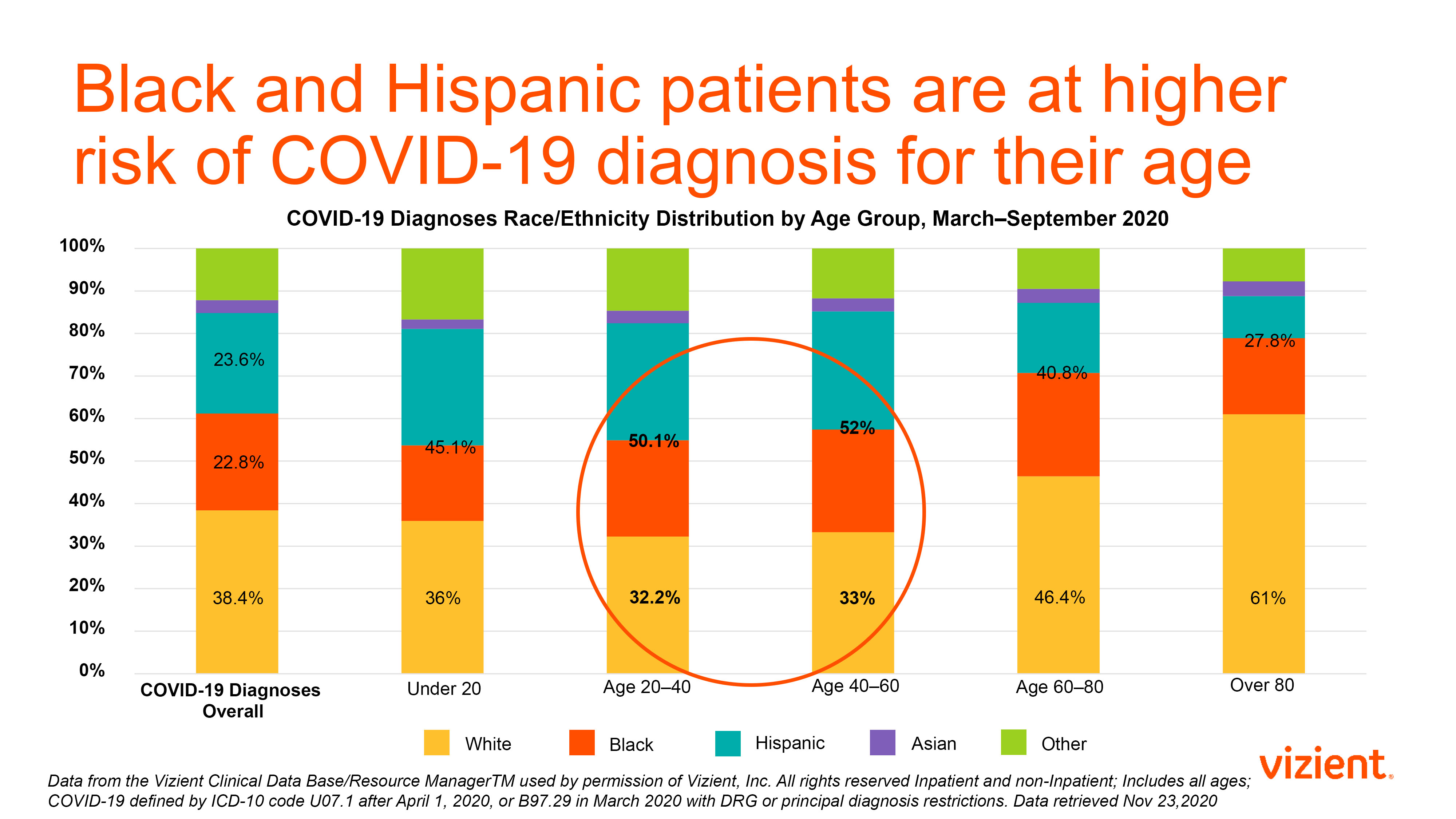
Finding your fit in addressing social determinants of health
Many hospitals and health systems do not feel equipped to tackle the often-complicated social determinants of health in their communities. These organizations have many strengths to offer community partners, such as technology and data analytics capabilities; clinical care expertise; project management talent; and in some cases, financial resources. It is true that not every organization is equipped to lead social determinants of health work, but every organization has an important role to play. And it starts with finding your fit.
We have developed a three-part framework for helping hospitals and health systems find their fit by examining their scope—the extent to which their ambitions converge with their financial, infrastructure and cultural capabilities.

Align—Some hospitals and health systems, while still tackling patient’s social needs, are also starting to address the social, environmental and behavioral needs of individuals beyond the medical setting. This phase is characterized by organizations acting as conveners to connect these patients not only to community resources such as food and housing, but also to develop closed-loop referrals in which the care team can follow the referral through that process. The result is a more tangible tie-in to cost savings and outcomes-based metrics. A great example is when a health care organization partnered with their local health center, care navigator organization and first responders to identify what support structures are needed to support a vulnerable homeless patient population and provide services upstream to help reduce high emergency department utilization.
Anchor—This phase goes far upstream of health care’s traditional role. Hospitals and health systems in this phase have begun to reframe their organizations not just as clinical care providers in their community but as community anchors, considering not only the essential clinical care the community needs but also recognizing the hospital’s impact as an employer, investor, purchaser and community partner. The organizations are working to make systemic changes to help revitalize not only the health of their patients but the overall health of their community as well. For example, there are organizations that have made commitments to things like $15 an hour wage for their employees. They may have commitments to hiring locally. They may have commitments to purchasing locally. They may take more active advocacy roles in changing local housing regulations, improving transit or promoting education.
COVID-19 has put a bright light on the impact of health disparities on individuals as well as on hospitals caring for those individuals and their communities. Conversations about the imperative of addressing social determinants of health is no longer about “why,” but about “how.” We are seeing really exciting change underway at organizations at every level of this framework.
We are at a very critical defining point to meet the unmet social needs and health disparities across the nation and in our communities. Not every organization is equipped to lead social determinants of health work, but every organization has an important role to play. Find your fit and start now.
More information about Vizient's work to advance health equity is available online.
About the authors


