by Gena Futral
Vizient Executive Principal, Reliability and Management Systems
Health care leaders frequently state their organization is on a high-reliability journey—but why? The simple explanation is the desire to have more reliable outcomes and overall performance. Achieving high reliability in health care though is a challenge due to the complexity and the dependency on human factors. The good news is that other highly complex and risk-prone industries have had success achieving high reliability and they provide great insights for health care organizations.

Health care organizations struggle with high reliability for various reasons:
- Leading based on high-reliability principles requires new roles and skills for senior, middle and frontline management.
- Systems and processes are unstable leading to variation and workarounds.
- Expertise is defined by title versus recognized by those closest to the work.
- Improvement science is knowledge limited to a select few.
- Harm events and missteps are managed punitively instead of as learning opportunities.
- Transparent data is not routinely shared as an accelerator to learning and improving.
- Culture and engagement data are not integrated with performance data to identify critical drivers to achieving goals.
- Organizational priorities are disconnected from daily work.
Transformation to high reliability is a journey, not a transaction. It can feel daunting for leaders and perhaps too theoretical. The approach for health care organizations can be “step-wise” and the good news is that any advancement will reap rewards for patients, families and the entire organization.
I don’t want to simplify this journey, as it is hard work and starts with leadership, but incremental transformation is possible and developing an informed and thoughtful plan that starts with a successful day one, is step one.
Four pillars essential for high reliability
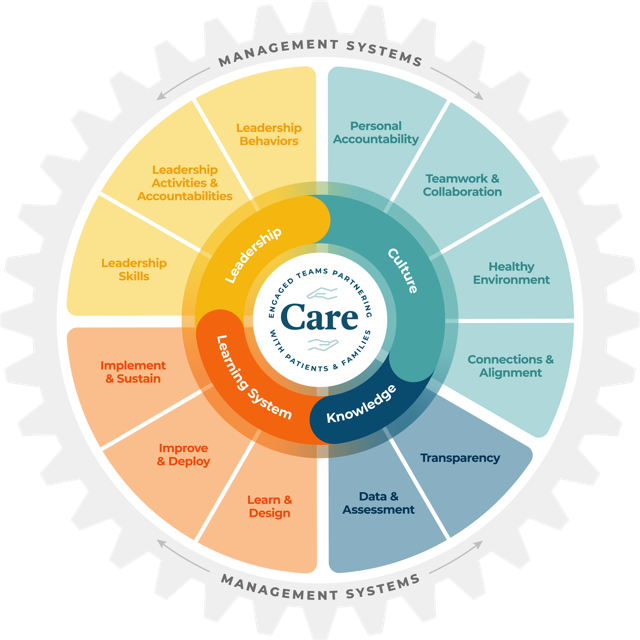
Pillar #1: Develop high-reliability leaders—Leading with communications and actions grounded in high-reliability principles is not innate. To support the transformation, high-reliability education is required along with individual coaching to adopt new practices into daily standard work.
Leaders at the executive, middle management and front line have different roles and each are individually important. Leaders must learn new skills to create an open dialogue, observe without judgment, coach improvement, problem-solve and facilitate change through visual management.
Pillar #2: Ground your culture in respect, collaboration and accountability—The organizational culture required to support the high-reliability transformation is developed over time and leaders are the cornerstone. Creating an environment based on respect for all individuals and ideas is the first step to developing trust and therefore safety.
For individuals to elevate ideas, present diverse thoughts, challenge the status quo and even authority, they must feel safe from negative consequences. Once the workforce believes, through actions and experience, they are safe to actively participate in and are critical to the transformation, their accountability as an individual and team matures. The focus shifts to a shared sense of purpose and accountability to achieve performance excellence for patients, families and then the organization.
Pillar #3: Gain knowledge through transparent and comparative data—A mature culture built on respect, collaboration and accountability are critical for an honest and transparent review of the qualitative and quantitative data that illuminate the organization’s strengths and opportunities. Clinical and operational data are critical for prioritizing opportunities and equally important is data that measures an organization’s culture of safety and employee engagement. It is the integration of these data points that provides a clear understanding of the current state and the levers required to achieve and sustain performance excellence.
Pillar #4: Support continuous improvement through learning systems—There is a science to learning and improving, and gaining the organizational skills to achieve improvements are critical competencies. A goal of high-reliability organizations is to create an army of problem solvers so organizations must assure there is competency and capability to assume this new responsibility. The adoption of improvement-science frameworks, tools and techniques is required to achieve a continuous learning and improvement mindset. These resources support various aspects of improvement such as root cause analysis, driver identification, small tests of change, measurement and variation identification.
Operationalizing high reliability through management systems
Deploying management systems grounded in high-reliability principles provides the infrastructure for executing organizational strategy, sustaining the results of improvement and creating a heightened state engagement. These systems are organized and led by those closest to the work and promote a continuous learning culture and improvement approach. Leaders actively engage based on their roles. Daily attention is given to improvement priorities, and open discussions occur to problem solve, innovate and share transparent data to understand performance towards goals. Management systems are foundational for improvement and critical to assuring sustainability is maintained after performance goals are achieved. They are the connection mechanism between the board room and the front line.
Embedded within management systems areas are the high-reliability principles defined by Karl E. Weick and Kathleen M. Sutcliffe in Managing the Unexpected: Resilient Performance in an Age of Uncertainty and perhaps the most recognized high-reliability organization reference. The following learned practices reinforce the high-reliability culture to continuously learn, build accountability, develop mindfulness and engage the entire workforce to be problem solvers:
- Preoccupation with failure—An appreciation for systems thinking and that the smallest signal requires a large response because the holes in the swiss cheese may be lining up.
- Reluctance to simplify—Health care is highly complex so all decisions and actions should be approached with skepticism, diverse perspectives and a willingness to challenge beliefs and assumptions.
- Sensitivity to operations—Understanding the gap between intentions and reality and appreciating how actions create ripple effects across interdependent systems
- Commitment to resilience—Organizational engagement for individuals and groups increases their ability to more effectively manage challenges and recover from events.
- Deference to expertise—Respect that those closest to the work are the experts and best armed to solve problems and develop impactful and sustainable solutions.
A high-reliability strategy provides an evidence-based and systematic approach to achieving and sustaining quality, safety, operational and financial performance excellence. It causes organizations to back up and look more holistically at how culture serves as a driver to performance.
By adopting high-reliability principles across the organization, from the board room to the bedside, a more mindful, respectful and trusting workforce emerges and new competencies and accountability for being a problem-solver are adopted.
Health care organizations are prioritizing high reliability because they see the positive impact on other highly complex and risk-prone industries and realize their historical approaches have had temporary success at best. They accept that health care has unique challenges but that only serves as an accelerator to the high-reliability health care transformation journey.
Earlier this year, Vizient announced the launch of its high reliability organization solution for sustained delivery of safe health care. Additional information is available online.
About the author
Gena Futral is responsible for solutions grounded in high-reliability principles that partner with organizations to develop leaders, transform cultures, embed management systems and enhance workforce engagement. Through her decade tenure with Vizient, Gena has developed and executed multiple strategic, operational and performance improvement solutions all aimed at supporting our members’ journey towards performance excellence. She leads four teams and each are critical to achieving high-reliability: analytics and improvement managers, accreditation advisors, patient safety organization and reliability and management systems.
