by Bradley Schultz
Vizient Principal, Reliability & Management Systems
In a recent blog post, my colleague Gena Futral shared how transforming to a high-reliability health care organization has become an organizational imperative and shared four pillars essential for high reliability. In this blog post, I’ll take a closer look at how health care organizations’ management systems provide the infrastructure for executing organizational strategy, sustaining improvements and creating a heightened state of staff engagement during the high-reliability journey.

While management systems are multi-faceted and, potentially, very complex, they can be summarized in three simple concepts: they create transparency, drive accountability and leverage problem-solving combined with continuous improvement to make things better.
Let’s talk about these a bit more.

Caregivers need to be able to see the connection between the organization’s vision and what it means for them in terms of specific behaviors. They then need to see the connection between the behaviors and processes involved in the work they do and the results or outcomes. When those connections are not clear, things simply do not make sense, and that state of mindfulness is very difficult to achieve.
Visual management is a very powerful tool that creates the ability to make these connections and develop a state of mindfulness to see the difference between normal and abnormal conditions and act on what they see to potentially avoid harmful events from occurring, now. It is, simply, impossible to tell normal from abnormal without first defining normal.
Visual management leverages visual media, sometimes in the form of electronic boards or other visual mechanisms, to convey unit performance information. The data that is shared often includes performance against strategic goals, process improvement activity and results, status and flow of work. This enables caregivers to “see” performance daily instead of getting it much later in the form of a monthly report.
Most harm-events are not the result of a single event, but rather a chain reaction of events. Being able to see that the first domino has fallen and knowing what domino to place your finger on to stop the chain reaction is central to the definition of high reliability. It is that mindfulness in action.
Driving accountability
In general, everyone in a health care organization knows what they are accountable for; however, to be effective, staff accountability must be interlocking with management and executive accountability, and the process must include coaching.
Accountability mechanisms are often referred to as “leadership standard work” (LSW). This standard is built from the frontline up, not the top down. It begins with reviewing a process—what are the most critical aspect of the process, the must-haves that define high-reliability performance? Those insights and performance measures are translated into a combination checklist and scorecard tracked by the frontline supervisor daily. Performance “misses” are addressed immediately. The scorecards are reviewed by mid-level management weekly and by executive leadership (via review of the mid-levels LSW) monthly.
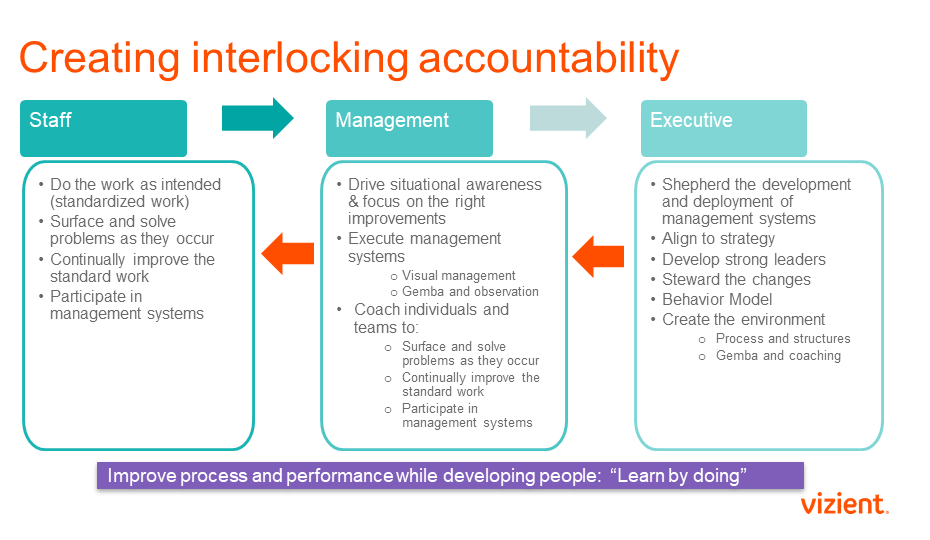
In a high-reliability organization that accountability isn’t just about performing the work as intended (standardized work). It also includes surfacing problems and continually improving the work. Interlocking accountability means that if these three things are not happening, the frontline supervisor is aware and is coaching caregivers to make them happen. If the frontline supervisor is unaware or not coaching, the mid-level manager is aware of that and coaching the frontline supervisor. Finally, if the mid-level manager is unaware or not coaching, their reporting executive is aware of that and coaching the mid-level manager. This applies to all aspects of accountability illustrated below.
Applying the concept of “standard work” to the accountability tasks of leadership is perhaps the most powerful tool when it comes to realizing the organization’s vision, high reliability or otherwise. It focuses on getting things right. It moves things out of the world of who “gets” it, into the world of who “does” it.
Leveraging problem-solving and continuous improvement
Every day, caregivers solve problems and develop workarounds for systems or processes that are not working appropriately. Working around problems can deter progress to high reliability and potentially cause harm. With workarounds, outcomes are no longer predictable (reliable), individuals may be less likely to find and solve the true root cause, and the longer a workaround is in place, the more likely it will ultimately lead to harm.
Have you ever participated in a process improvement initiative, see things get better, but then see the workflow slowly drift right back to where it was before the work started? That’s the number one complaint I hear from caregivers at all levels: we are fixing the same things over and over again.
As I dig into it, I learn that their management systems have not created adequate transparency for them “see” the break or driven the interlocking accountability required for disciplined adherence to the new process. As a result, it is abandoned at the first challenge within the new process. High-reliability organizations understand and embrace the problem-solving and continuous improvement that must be included in any process.
Typically, systems or processes don’t work for three reasons: a standard does not exist, performance does not meet the standard or the standard needs to be tightened. Most of us are familiar with the second reason. Few, however, give equal consideration to reasons number one and three. Without a standard, there’s no way to tell normal from abnormal and take immediate, appropriate action. Also, the routine tightening of standards exposes next-level problems, which is the essence of continuous improvement or kaizen.
The overarching objective here is to create an environment where problems, and workarounds, are not tolerated. This requires building problem-solving capability in every employee. Leveraging visual management to make the abnormal stand out, acting immediately, and using the scientific method to prevent recurrence completes the cycle.
To sum it all up, management systems are foundational for improvement and critical to assuring sustainability is maintained after performance goals are achieved. They are the connection between the board room and the front line, making vision actionable.
Earlier this year, Vizient announced the launch of its high reliability organization solution for sustained delivery of safe health care. Additional information is available online.
About the author
Bradley Schultz assists Vizient members in making large-scale, transformational change within their organizations using Lean, Six-Sigma, High-Reliability-Systems Design and other proven methods resulting in dramatically improved operating performance. He partners with members to architect the change, plan and coach the implementation. Bradley has more than 25 years of consulting and executive coaching experience, primarily within the health care industry. Prior to joining Vizient, he spent four years as vice president operations & quality for a $160M multi-channel merchant. This was preceded by 20 years with GE as a manufacturing engineer, operations leader, health care consultant and regional consulting practice leader.