Among the hot topics in health care right now is the concept of service distribution — the hard work that health systems are doing to ensure that services are appropriately placed across the system’s various facilities and campuses to meet patients’ needs now and in the future. In some markets, or with select services, this may mean service expansion, such as enhancing access to virtual health, primary care or rehab, but often this translates into service consolidation (e.g., centralizing orthopedics from multiple acute facilities to fewer).
“The aim is to shift a hospital’s identity from within a community to within a system, all the while ensuring that patient touchpoints remain intact in an effort to reduce risks of leakage,” said Lisa Slama, PhD, associate principal at Sg2, a Vizient company.
The path to service distribution
For many organizations, a wide range of forces, both external and internal, are making service distribution planning worth the time and effort — if not compulsory. This type of planning entails a reconsideration of which services are being offered across the enterprise and where. In markets with growing populations, redistribution efforts can expand access channels for key services to stay ahead of competitors. In flat or declining markets, service restructuring can reduce redundancies and enable efficiencies that drive down costs.
External factors such as demographic changes or actions by employers, payers or competitors often necessitate a rethinking of the organization’s portfolio. Within the organization, integration after a merger or acquisition is a frequent driver of service distribution planning.
“The growth of the system itself may be a trigger: some systems have become so large that they are difficult to manage. In such cases, new organizational structures may need to be put into place before comprehensive service distribution planning can be done,” continued Slama.
A long-postponed enterprise decision about a new facility also frequently spurs a reexamination of the optimal breadth and location of core clinical services. So may new management structures for ever-growing medical groups. Even the organization’s regular review of the master facility plan may prompt a broader, more strategic look at all facilities and services. Thus, savvy architectural and facility planning firms will push their health system clients to consider new options.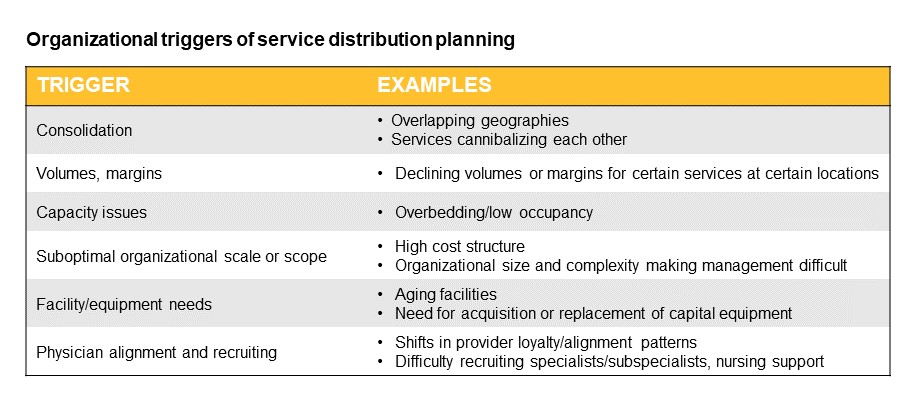
The broad range of market and organizational triggers make it likely that service distribution planning will be essential at most health systems in the near future. The question is likely to be not whether to do service distribution, but when, and how extensively. In fact, service distribution is a topic strategic planners and service line leaders should review on a regular basis.
Systems that have done this work successfully have gained economies of scale, boosted performance, lowered costs and simplified decision making regarding future investments. Although this work can improve the value of care across the system, it also comes with incredible risk. These projects are long — often taking a year or more — and require heavy lift to move, consolidate or eliminate services across sites within a large system.
The high stakes often push hospital executives to pump the brakes when it comes to making these big, bold decisions. “Without an effective way to evaluate service placement options, the analyses fall short and efforts get derailed,” said Slama.
For one organization we spoke with, a change in system leadership disrupted their project’s momentum and, without rules and a clear plan, the efforts were tabled indefinitely. Another organization lacked a clear communication plan regarding possible service changes. This led to rumors across the staff and community at large that were significant enough to scrap the entire project.
Unfortunately, derailments like these are more common than not and force organizations to stick with their current, distributed service model — the status quo. This shortsighted approach resists service disruption but fails to set up most markets for the long-term success enabled by a model that reduces cost without hindering quality or patient access. A well-constructed service distribution strategy includes a strategic, objective evaluation process.
Effective service distribution is implemented in stages
The key stages of service distribution are outlined below and make up a systematic, data-driven approach.
- Assess feasibility, gain commitment: Confirming the organization’s ability and political appetite to follow the process to its conclusion is essential. A key first step is to form a small, trusted team that can answer the tough questions around the project rationale, scope and timing, along with its financial, political and community implications. This team will be tasked with cataloguing current offerings, provider capabilities and performance by facility and ultimately reaching a go/no-go decision.
- Evaluate a range of configuration options: Once the decision is made to move forward, the next phase is to integrate impartial criteria and a data-driven process for decision making. Identifying the guiding principles and setting ground rules help keep the process objective and rational, rather than politically charged. Guiding principles should stem from the organization’s vision and goals and serve as a way to objectively evaluate all options
During an Sg2 Executive Summit panel discussion, Dr Tim Babineau, president and CEO of Lifespan in Rhode Island, stressed the importance of establishing the right selection criteria when his system set out to evaluate a centralized model for cardiovascular surgery, saying “It took six months to create and agree upon our guiding principles, but it helped to get everyone on the same page and was a main driver of why we were able to move cardiovascular surgical services from two facilities to one.”
- Communicate and implement the decision: Each strategy will require a unique implementation plan — a road map including key milestones and clear, ongoing performance metrics and financial targets. When communicating the plan to stakeholders, present the facts supporting the new configuration and the timeline for redistribution. Gain stakeholder buy-in by emphasizing how the plan will support long-term enterprise goals.
An effective implementation plan aligns senior leader incentives so they are based on the success of the entire enterprise — not on campus-level performance. For example, a hospital CEO whose incentives are based on market share and margins at his facility will not be likely to support a plan to move high-margin services to another one.
Dr. Greg Bazylewicz from Lahey Health spoke at an Sg2 Executive Summit of the importance of realigning incentives as Lahey prepares for a major systems merger. “Ensuring that we have a plan to incentivize our leaders across various facilities based on system goals, rather than individual facility goals, will be important to our overall need to reduce cost and provide the highest-quality care.”
Resist the status quo
With a carefully constructed plan, service distribution work allows organizations to objectively evaluate configuration options with the goal of creating a stronger, financially viable system optimized for long-term growth. The above 3-stage approach is designed to keep the team on track, evaluate various options, and leverage data and organizational goals to ultimately make the best choice. Slama concluded, “Done correctly, it allows organizations to hone in on the right service configuration model and resist the status quo when the data suggest otherwise.”
Sg2 can help guide organizations as they consider the optimal distribution of services to achieve scale across the care continuum. For more information, explore Sg2's various service distribution resources or contact Sg2 directly.
Sources: Sg2. Service Distribution: Making the Hard Choices. 2017; Sg2 Analysis, 2017-2019.
