by Roseann Hoeye, Vizient Director, Nutrition and Environmental Services Advisory Solutions
Bridget May, Vizient Product Executive
It sounds simple, but one of the secrets to success for food service managers is to know your business. Food service managers are challenged every day to justify spend, capital investment, manpower and productivity. A solid benchmarking process that is adaptable and can be maintained will provide you with an understanding of where your hospital fits within today’s competitive market as well as the data that’s needed to make the best decision for your hospital. Both are critical to your conversations with hospital leadership.
Here’s four steps to ensure your food service benchmarking process is optimized to provide the most valuable information that you need for your stakeholders.
Develop your benchmarking plan
Benchmarking provides focus in your department’s quality management program. Include your employees in the plan. You need their support. The inclusion of benchmarking, metrics and measurement also creates another tool for communication with administration. Having facts and figures as part of the plan provides you with the backup you need to make improvements in equipment, service or additional employees.
Your plan provides the essential framework for success. It can be a product, service, practice, or total department review (including food, operational or labor costs). Here’s a few high-level questions to help formulate your plan:
- How well are we performing compared to other food service operations?
- What are the best practices?
- What improvement opportunities should we focus on?
Identify and collect key data
Based on the goals and objectives of the plan, and leveraging the nine key metrics that define the foodservice department (see sidebar), ask yourself:
- What data am I looking for and what sources are needed?
- Where will the data come from and who will collect it?
- How often will the data be collected?
- How do I know the data is accurate?
Analyze and interpret the data
Benchmarking tools can provide guideposts and data to compare your hospital to industry norms as well as general competitive information. There’s a variety available, including from professional organizations and distributors as well as enterprise-wide subscription-based tools. Be sure to understand how they define data elements and ensure you are reporting consistently.
Determine your cost per patient day (PPD) and cost per meal (PPM). PPD = net cost/patient days and PPM = net cost/number of meals. Many consider PPD as the best measure of high versus low cost and the most reliable measure, and consider PPM as a good measure for determining actual savings during times of decline or growth related to patient days or meals and efficiency for meals. Looking at these numbers together, however, provides deeper insights.
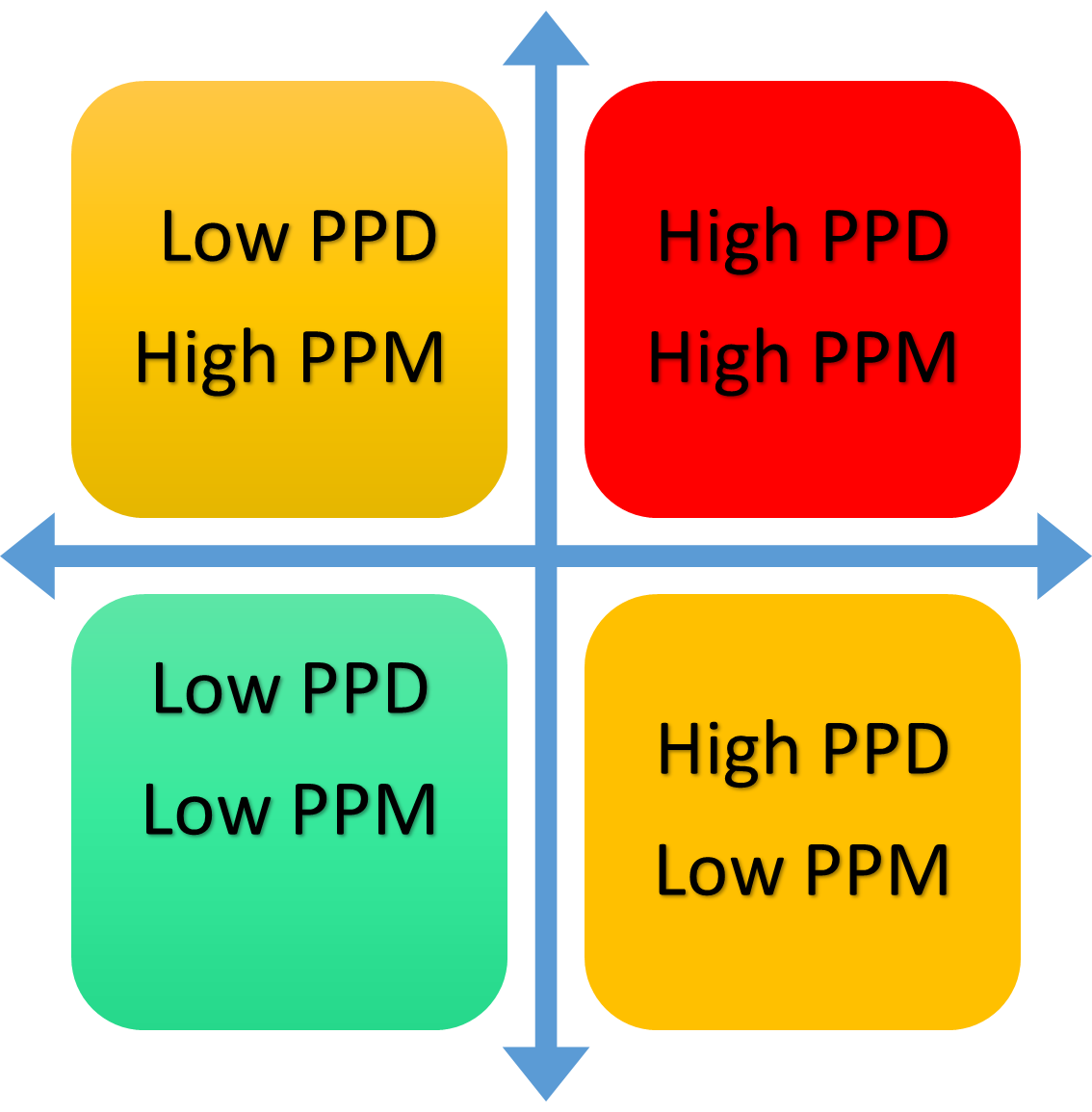
- Low PPD and low PPM indicates a strong position. Maintain this through a focus on managing costs as well as quality and patient satisfaction.
- If you have low PPD and high PPM, there’s room for improvement. Focus on greater efficiency and lowering menu and labor costs.
- High PPD and low PPM may indicate strong management but too much subsidy to the operation. Consider reviewing floor stock as well as catering, cafeteria pricing and non-patient feeding.
- High PPD and high PPM indicates opportunity to improve in all areas. Consider a review of efficiency, labor costs, non-patient feeding, product standardization and selection, and overall food costs.
Develop an action plan to improve performance
Now that you’ve completed your benchmarking, identified and interpreted important data points, it’s time to develop an action plan designed to either improve or maintain your program. Your action plan should be detailed with steps and a timeline showing how and when it will be implemented, who will be responsible and how it will be monitored.
Be sure to communicate with the appropriate team members on the purpose of your benchmarking goal and establish a task force to aid in the implementation. Stay connected with organizations that provide benchmarks you will use in your plan to evaluate your progress and stay current on new trends.
Now that you’ve created your strong hospital food service benchmarking process, don’t stop. Continue to educate, innovate and advocate. Continue to educate on quality management program, innovate new programs and services in your department, and advocate for your department performance and employee engagement.
Benchmarking should be a continuous improvement journey that builds on past successes, failures, and lessons to keep your department or organization evolving and meeting the needs of its stakeholders in the best possible way.
Learn more about Vizient’s food service offering on our website.
About the authors
Roseann Hoeye, MBA, RD, LD, is senior director, nutrition & environmental services advisory solutions. Roseann earned her Bachelor of Science in Dietetics from New Mexico State University and a Master of Business Administration in Healthcare Management from the University of Phoenix. She consults closely with members to maximize contract utilization and cost savings as well as advising on operational and financial nutrition and environmental services subjects. Her previous experience includes roles in acute-care, long-term care, community nutrition, home health, corporate wellness programs and physician offices.
Bridget May, MA, RDN, FAND, is a product executive with Vizient Inc. She is a registered dietitian nutritionist with an MA from Webster University. Her career encompasses more than 20 years of clinical and food service operations in acute care facilities, followed by an additional 20 years in the group purchasing industry. Bridget joined the legacy group of Vizient companies in 1998 and has played numerous roles within its food program. Her varied background and lifelong learning support her current role in both member-facing and supplier-facing efforts as well as food program communications, education opportunities and event coordination.

