In its annual Impact of Change® forecast, Vizient’s subsidiary Sg2 projects a strong recovery for overall patient demand that will surpass 2019 volumes. While this is welcome news for an industry that has been reeling for the last 18 months due to an array of challenges related to the COVID-19 pandemic, digging into the details shows trends that will require shifts in resources and investments by hospitals.
“Hospitals are understandably focused on short-term pandemic recovery timing and what that looks like by service line,” says Maddie McDowell, M.D., principal and medical director of Sg2. “At the same time, long-term strategy and planning are needed to prepare for site of care shifts, technology advances that impact service offerings and the growing chronic disease and aging population.”
The report details short-, medium- and long-term trends in several key areas:
- Inpatient admissions: Inpatient volumes will decline over the next 10 years as patient acuity rises. The growth of outpatient surgery volumes and hospital at home programs are fueling the decline. An aging population and increased demand for tertiary care will contribute to inpatient growth.
- Surgical site shifts: Surgical volumes will continue to move out of the hospital to the hospital outpatient department (HOPD), ambulatory surgery center (ASC) and provider offices/clinics. The outpatient surgery growth is due to a combination of factors, including the Centers for Medicare and Medicaid Services relaxing site restrictions, clinical innovations and private equity investment in ASCs.
- Emergency department visits: After a 20 percent decline in emergency department (ED) volumes last year, expect a short-term rebound. Over the next 10 years, overall ED volumes will drop by 5 percent.
- Outpatient care: By the end of the decade, 30 percent of all evaluation and management visits will be virtual, contributing to a 19 percent drop in in-person visits. Diagnostic and procedure volumes are projected to grow 18 percent by 2029.
A deeper dive into the trends
Lower inpatient volumes, sicker patients—While inpatient volumes for elective procedures is rebounding quickly as the level of COVID-19 infections declines, demand is unlikely to surpass 2019 levels. Through the end of the decade, overall inpatient volumes will remain flat, while tertiary care will grow by 16 percent. ICU demand is also projected to increase.
These inpatient trends reflect 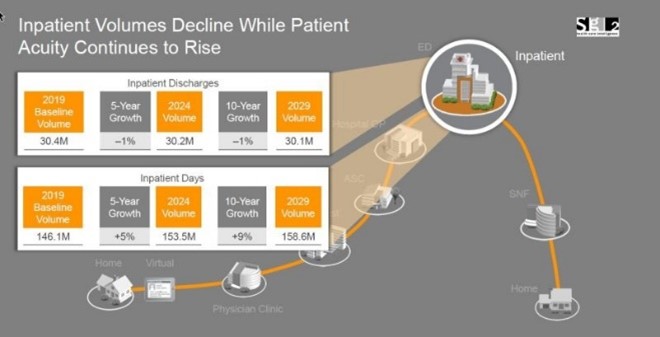
Additionally, the pandemic catalyzed health systems to rethink care for conditions such as congestive heart failure and COPD and opened the door to innovative home care models. In the latter half of the decade, scaled hospital at home programs will increasingly be used to offset inpatient demand for medical admissions , fueled by CMS payment pilots, advances in remote monitoring and demonstrated improved outcomes and lower costs. Overall care in the home is projected to grow 15% by 2029.
Surgical site shuffle—Through the rest of this decade, outpatient surgery volumes will continue to grow exponentially: hospital outpatient department (19 percent), ambulatory surgery centers (25 percent) and physician offices/clinics (18 percent). Key service line trends include:
- Cardiovascular care: An overall increase in this disease will continue to drive demand for services however, most procedures will remain in the hospital setting. Higher acuity procedures, such as coronary artery bypass grafting and valve replacement, will stay in the inpatient setting. Pacemakers, implantable cardioverter defibrillators and other electrophysiology procedures will largely remain in the hospital outpatient department. Ambulatory surgery centers will receive a rising share of vascular procedures and over time, a small proportion of diagnostic catheterizations and percutaneous coronary interventions will migrate there.
- Orthopedics: The shift for procedures to the hospital outpatient department and ambulatory surgery centers will accelerate as CMS evaluates which procedures will be removed from its in-patient only list (more than 1,700 codes). By the end of the decade, only 20 percent of total joint replacements are expected to occur in the inpatient setting.
- Neurosurgery: Neurointerventional procedures represent a bright spot on the inpatient horizon. Expanded applications of neurointerventional procedures, such as thrombolytic therapy, carotid angioplasty and endovascular coiling, will improve outcomes and boost inpatient volumes over the next five years.
ED volumes rebound but below 2019 levels—After a year of consumer reluctance to use the emergency department combined with lower infectious disease rates due to masking and social distancing, ED volumes will rebound over the next three years but stabilize below 2019 levels. Emergent visits are expected to increase 5 percent over the next 10 years, with behavioral health, chronic disease care and cardiovascular visits contributing the most to the growth. Low acuity ED visits will drop by 15 percent as these volumes continue shifting to urgent care centers and other alternative sites of care.
Outpatient virtual care is here to stay—Patients who delayed or deferred care during the pandemic and COVID-19 “long haulers” are contributing to increased, short-term demand for both in-person and virtual visits. By 2029, while evaluation management visits overall are expected to grow, in-person office visits are projected to decline 19 percent due to the growth of virtual care.
The pandemic provided a view into which conditions and service lines were best suited for virtual visits. By the end of the decade, nearly one in three appointments will occur virtually, with behavioral health (50%of visits being virtual), medical specialties (37% virtual) and neurosciences (31% virtual) leading the pack.
“By the end of the decade, we predict patients will be seeing providers in new, very different ways than they used to,” says Dr. McDowell. “Members should begin planning for future clinic space needs. Does the space include a virtual hub so providers can alternative between in-person and virtual care? Do you downsize your square footage to a smaller footprint or repurpose the space for virtual services and higher acuity patients?”
Prepare now for the transformation of care delivery
Rising patient acuity and an aging population will have significant facility, workforce and financial implications for health systems. In addition, clinical innovation and evolving payment models are rapidly transforming care delivery. “Having an understanding the of what health care could look like in five or 10 years is so important because health systems have to start preparing and investing now,” adds Dr. McDowell.
As health systems navigate post-pandemic recovery, they should begin to think about planning for volumes to shift to lower-cost sites of care, opportunities to invest in chronic disease management services and their ambulatory footprint and strategy.
Additional insights from the forecast are available from the Sg2 Perspectives podcast.
