Elizabeth, or Libby as her friends and family call her, has been a fighter her entire life. Born with kidney and lung problems, her battle began very early. Doctors in the neonatal intensive care unit didn’t expect Libby to go home but eventually she did. After several months of home dialysis, special food preparation and challenging care, Libby was strong enough to receive one of her mother’s kidneys.
Throughout the years since then Libby has fought long and hard to keep that kidney functioning. Her life involves regular doctor visits to ensure the kidney was not being rejected. She has taken as many as 10 pills a day and, because she’s also developed type 1 diabetes, she has had to endure several finger sticks and three to four insulin shots each day. This was Libby’s “normal.”
In 2017 Libby graduated from high school. She started taking classes at the local community college, and was enjoying her new home in Florida. In October 2018 during one of her regular check-ups, her lab results came back abnormal. There wasn’t any indication of rejection, so she went home to be re-checked at a later time.
During the follow-up visit, she was found to be battling four to five infectious diseases and was hospitalized. After 10 days in the hospital she was discharged, only to return to the hospital two days later with pain at her transplant site. The doctors worked hard to find the right balance of medication to fight all of the infections and to save her kidney. She went home after another week in the hospital.

After they arrived, things happened quickly. Within the first hour they had her history and vital signs, started an IV, did blood cultures and started antibiotics. When her father asked about sepsis, the doctor replied that Libby was already in septic shock, a very serious situation. Going into that first night the physicians told Libby’s parents that they needed to prepare for the worst. Libby and her body were undergoing another fight of their life. Miraculously, her body responded to the antibiotics and her blood test results started to rebound.
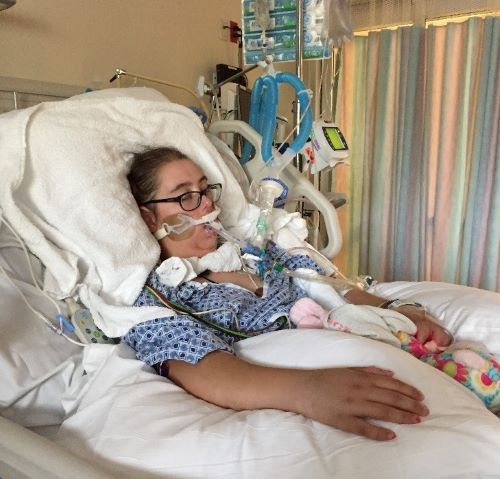
Libby’s father wants to share that each of us need to remember “carpe diem,” i.e. seize the day. Each year Libby and her family celebrate the day of her kidney transplant. This year they have even more to celebrate. Libby is looking forward to having her favorite Thanksgiving foods which she missed last year.
If you experience these symptoms and suspect sepsis, act quickly to get treatment. If you have been diagnosed and treated for sepsis, recovery is long and may result in serious consequences for several weeks after being treated.
The U.S. Centers for Disease Control and Prevention (CDC) recently launched a new website to increase sepsis awareness, and improve early recognition, diagnosis and treatment. The Surviving Sepsis Campaign includes evidence-based guidelines, performance improvement initiatives, and analysis and publication of patient data.
If you are interested in learning more about the sepsis-related projects offered through the Vizient PI Collaboratives Program, contact us today.

