- Clinical
- Operations & Quality
Nurturing success: Retaining strategies for newly licensed nurses
In a recent focus group, the Vizient/AACN Nurse Residency Program team uncovered themes that contribute to high levels of support and professional satisfaction, most notably providing stable transitions and creating a healthy work environment.
- Supply Chain
8 (mostly easy) ways to reduce your medical gas spend
As health systems continue to navigate tight margins and seek ways to transform variable expenses, there are some quick wins to be found. Step No. 1? Understand your product supply agreement.
- Clinical
- Supply Chain
Four ways to address ligature risks in patient rooms and beyond
Ligature risk mitigation requires collaboration among stakeholders and adherence to best practices, including comprehensive risk assessments, implementing design solutions, staff training, and ongoing monitoring and evaluation.
- Clinical
- Pharmacy
- Operations & Quality
A Chief Pharmacy Officer in your C-suite: Vital to health system success
Margins are tight everywhere in healthcare, but a hospital’s pharmacy department has a strong capacity to bring value — especially if that organization has an established chief pharmacy officer as part of its C-suite.
- Clinical
- Operations & Quality
How do you compare? Leverage data to optimize your payer positioning and value-based care performance
Vizient’s Tawnya Bosko outlines five strategies for how healthcare providers can use claims, clinical data and benchmarking services to maximize their potential with payers by navigating blind spots and refining improvement efforts.
- Supply Chain
Tap into these four strategies to improve hospital water quality
To ensure patient safety, water quality is key. And there are four main strategies that can help achieve that goal: regular water quality testing, water treatment and technologies, equipment maintenance and calibration, and education and training.
- Operations & Quality
Think Like Tech: Lessons for Healthcare Organizations
Is your healthcare organization keeping up with the pace of change? In a world of digital disruption, it's time to think like tech companies and embrace innovative strategies. Explore further insights in Vizient CEO Byron Jobe’s latest blog.
- Clinical
- Operations & Quality
Value-based care disruptors: What can health systems learn from their successes and failures?
By paying attention to how value-based care disruptors are changing the healthcare landscape, system leaders can adapt to their own strategies to share in the reward of increased patient quality care and service at a lower cost.
- Clinical
- Operations & Quality
Improving patient safety: Early recognition and a timely response to clinical deterioration
Vizient’s Tammy Williams shares recommendations on how healthcare organizations can improve patient safety with timely response to clinical deterioration.
- Clinical
- Operations & Quality
Implementing trauma-informed care: A tool to prevent violence in healthcare
Trauma-informed care can be a successful strategy for healthcare organizations to prevent violence by integrating person-centered strategies that prioritize safety, minimize triggers and promote empathy and mutual respect.
- Supply Chain
One size does not fit all: The power of customer segmentation
In today’s highly competitive healthcare landscape, companies that embrace tailored segmentation approaches have witnessed significant gains in sales efficiency and profitability.
- Pharmacy
- Clinical
- Operations & Quality
Navigating the laboratory’s macro- and microeconomic environment
Amid a macroenvironment of inflation and rising healthcare costs, healthcare leaders should carefully assess these microeconomic trends as part of their hospital-based laboratory decision-making throughout 2024 and beyond.
- Clinical
- Operations & Quality
It's Time to Refresh Your Value-Based Care Strategy: Six Trends to Consider
To remain relevant in all aspects of healthcare financing and delivery, leaders should evaluate their value-based care strategies to consider key trends and market conditions.
- Pharmacy
Drug Shortage Stewardship: Calls to Action for the Interconnected Supply Chain
While the supply chain may feel complex, the good news is that there are still methods — like Drug Shortage Stewardship — that can be implemented to mitigate drug shortages.
- Clinical
- Operations & Quality
Community Health Workers: A Bridge to Health Literacy and Patient Outcomes
With a deep understanding of the communities they serve, community health workers are significant resources for healthcare organizations to improve patients’ health literacy and address their clinical and non-clinical needs.
- Supply Chain
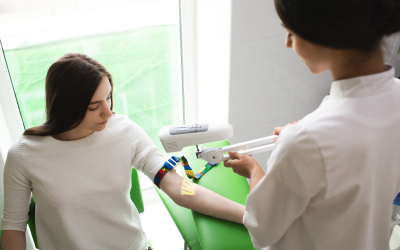
Vein Viewers Offer Benefits for Patients and Providers
The devices can reduce the discomfort and pain associated with multiple attempts at finding a vein and improve the accuracy and speed of vein location, reducing the need for repeat attempts or more invasive procedures.
- Clinical
- Operations & Quality
- Supply Chain
Improving the Provider Narrative: Vizient's Briefings Amplify the Voice of Hospitals on Capitol Hill
Learn about the three briefings that Vizient hosted in 2023 — attended by dozens of Congressional staff and Members of Congress — serving as a platform to remind policymakers of the critical impact of hospitals and health systems in their communities.
- Clinical
- Operations & Quality
In Healthcare, Culture is Where Margin Meets Mission
Creating a 'glad to be here' culture in healthcare is more than just a motto. It's a mindset that drives excellence and exceptional care. Learn how to merge margin and mission in your organization in the latest blog post from Vizient CEO Byron Jobe.
- Data & Analytics
Consumer-centricity: Reorienting Your Growth Strategy to Focus on Patient Loyalty
To ensure healthcare organizations remain competitive and financially viable, they must learn to build patient loyalty to create long-term relationships.
- Clinical
- Operations & Quality
Reviving the Nursing Workforce By Applying Starling’s Law
Learn how healthcare leaders can work together to optimize systems to ensure nursing’s trusted place in delivering high-quality, patient-centered care — without missing a beat.
- Clinical
- Operations & Quality
Investing in Advanced Practice Provider Transition to Practice Programs
As nurse practitioners and physician assistants play an increasingly crucial role in bridging healthcare gaps, the need for organizations to implement transition to practice programs is paramount.
- Clinical
- Operations & Quality
Using Social Drivers of Health to Reduce Admissions for Diabetes Patients, Among Others
By leveraging the patent-pending Vizient Vulnerability Index™, healthcare organizations focused on mission and margins can act upstream to directly address SDOH to help reduce preventable admissions in high-needs communities.
- Clinical
- Operations & Quality
Letting Go of Past Prized Practices: Making Meaningful Change in Healthcare
To address the struggles in healthcare, healthcare organizations must be willing to shift their mindset, challenge the status quo of old practices and embrace meaningful change.
- Supply Chain
- Clinical
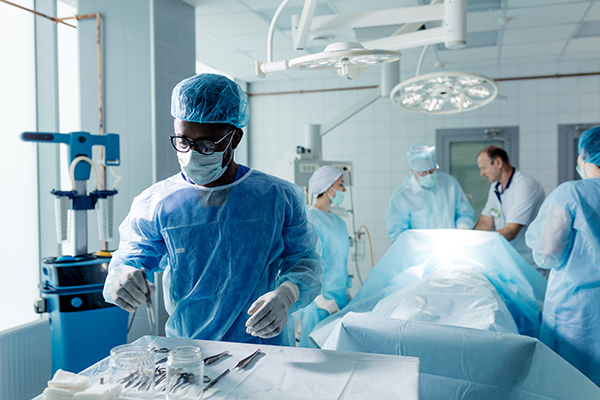
Principles of Surgical Tray Management: How to Save Time, Effort and Money
As hospitals and health systems work to manage costs while maintaining care quality, surgical tray standardization remains an untapped opportunity for many organizations. But there are ways to streamline instruments and provide additional value.