by Kristi Biltz, CMRP, Vizient Consulting Director
Cheryl Poplaski, Vizient Vice President, Supply Chain Operations
Clinical value analysis, in its essence, is a decision-making platform where the clinical value analysis team pulls data and information from various sources to tell a story around the initiative at hand. Most health care leaders believe their hospital supply chain and clinical strategy teams are working in alignment to achieve organizational goals for cost and quality of care. However, in our experience that is often not the case.
Instead, miscommunication and confusion about roles, responsibilities and processes creates an inconsistent or inefficient approach to performance improvement initiatives. Through our work with a wide range of hospitals and health systems, the supply chain and clinical value analysis teams that are most successful at collaboration use a common set of best practices.
- Establish roles and responsibilities—The ability of clinical value analysis and contracting teams to pivot between initiating and supporting the different aspects of the value analysis process is vital. Establishing roles and responsibilities is key to avoiding confusion and territory battles that can distract staff and derail the two departments. For example, defining who is the primary lead in discussions with the supplier eliminates duplicate conversations that can disrupt the negotiation leverage.
The supply chain team is responsible for delivering a vital portion of the story: the contract summary. This is the full contract history for a particular product or category. It also includes pricing, potential conflicts, group purchasing organization (GPO) v. local contracting strategies, vendors, new technology assessments and new product requests. Contracting also initiates assessments when contracts are expiring, or compliance is in question.
The clinical strategy team is responsible for providing clinical preference information related to procedural outcomes and facilitating physician engagement when product categories are evaluated. For example, when reviewing a urology product category including the physicians in the discussion with clinical value analysis and contracting allows each area to provide insights.
Additionally, clinical value analysis and contracting teams should share communication responsibilities; however, assigning various communications to an owner prevents confusion and sets expectations across the teams for who owns each of the communications during the initiative and prevents duplication and mixed messages.
When this information is brought together, and effectively communicated, it provides the clinical value analysis committee with the necessary tools to drive decisions.
- Use strategic sourcing tools—A variety of strategic sourcing tools can play a critical role in the success of pulling the teams together. These tools include working together to develop an annual work plan, a process map that clearly defines handoffs and a contracting decision tree that is shared across the clinical value analysis committees
Developing an annual work plan is necessary to effectively lead the teams, assess workload and prioritize projects. The work plan should include at minimum, the following items:
- GPO and local contracting calendar—includes information on products, vendors and contract length and expiring categories
- Identified savings opportunities
- Product and service evaluations
- Clinical need
- New technology and new product requests
- Quality initiatives
- Practice standardization/utilization goals
- Scoring platform to prioritize clinical need (it also enables management teams to set expectations, communicate timelines associated with end-user requests and plan staffing needs)
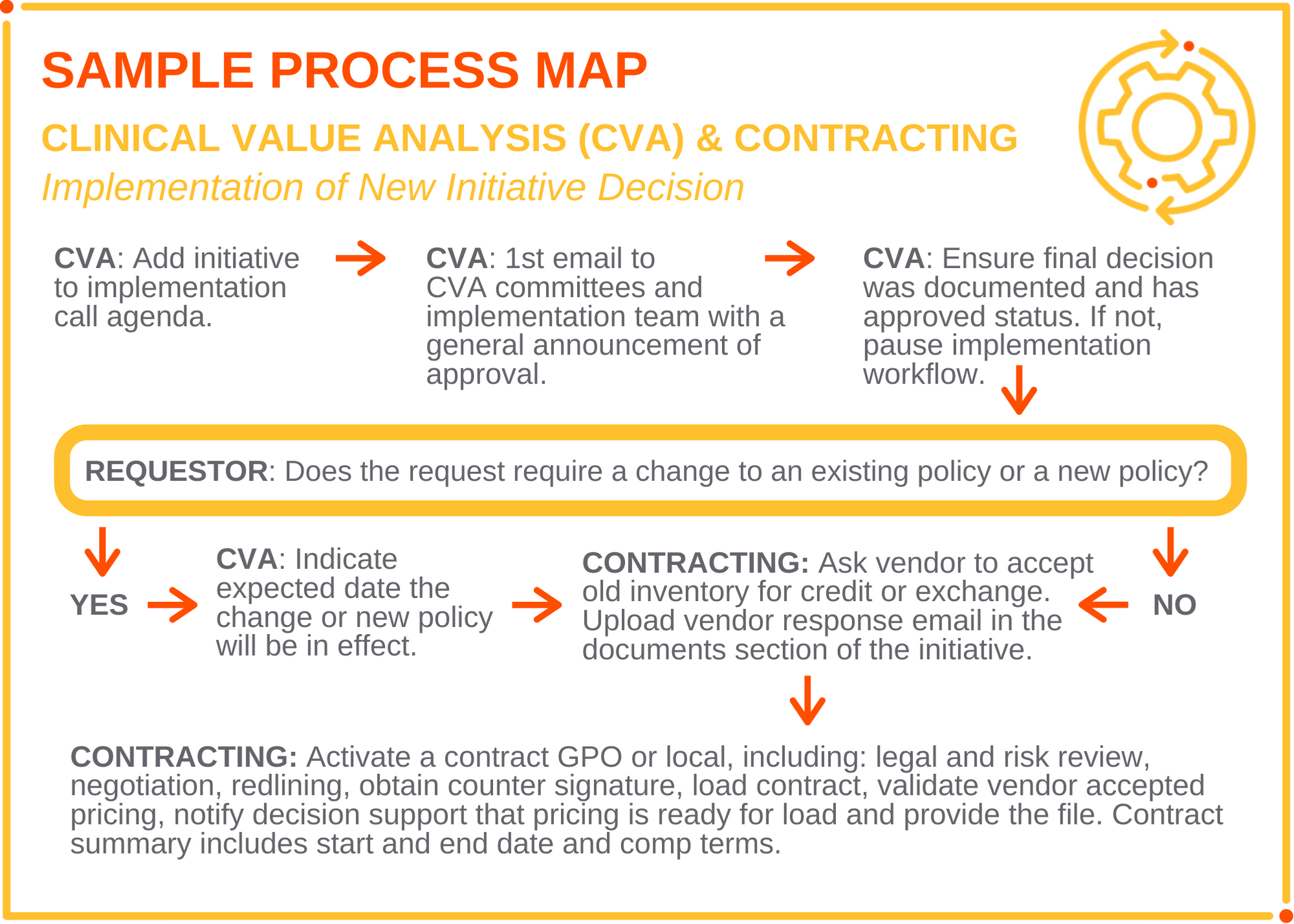
Another key tool is for supply chain leadership to develop and distribute a decision tree to staff. This assists them in evaluating how to approach a clinical value analysis project. For instance, should they align with an existing GPO agreement or is it more beneficial to the organization to pursue a local contract. The decision tree can be based on a variety of factors, including spend, savings, increases, categories, GPO versus local, mandatory terms and conditions (versus negotiable), clinical evidence, physician feedback, trials/evaluation results, market share and new technology.
- Develop a communication plan—It is impossible to overstate the importance of a clear communication plan developed jointly that provides updates to relevant committees, end users and other stakeholders involved in the initiative. You will want to decide and communicate upfront the expected frequency of correspondence. In addition, consider the following when developing your plan:
- Communication channels—Ensure you take advantage of the various communication channels available and create those that are not available. As an example, some hospitals use huddles. Creating high-level communications that can be shared in a huddle would be a valuable way to take advantage of an existing communication channel.
- Communication formats—Decide what types or styles of communications will be most useful to the teams. Examples include formal memos, informal emails, etc.
- Communication style: Keep your information relevant to the audience to prevent communication fatigue. Communications should be informational and action-oriented with specific direction and timelines.
A strong working relationship between the clinical value analysis and contracting staff is critical to ensure alignment between supply chain and clinical strategy teams, and ultimately, the success of the overall initiatives. This cannot be taken lightly as the quality of the initiatives are also tied to patient outcomes.
Aligning staff members into working teams so that they share goals and objectives and can work a project from various perspectives with seamless handoffs, can bring a total value package where cost, quality and outcomes are impacted in a positive manner.
About the authors
In her role as consulting director on the clinical advisory team, Kristi Biltz, CMRP, uses her more than 25 years of experience in the health care industry to assist acute care hospitals consistently integrate clinical and supply chain data in a clinical value analysis setting. She helps hospitals improve practice and product variation through a standardized decision-making process supported by evidence and best practice within a culture of continuous process improvement.
Cheryl Poplaski has more than 30 years of experience in all areas of supply chain and is particularly effective in implementing systems and redesigning operations to increase efficiency and reduce cost. Cheryl serves as Vizient’s vice president, supply chain operations. She joined the Vizient team in August 2001 and during that time has served in various outsourced supply chain leadership capacities at a number of member organizations, overseeing day-to-day operations as well mentoring staff and advising on process improvement.
